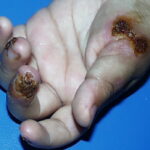
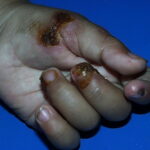
Electric burn
Electrical injuries, although relatively uncommon, are inevitably encountered by most emergency physicians. Adult electrical injuries usually occur in an occupational setting, whereas children are primarily injured in the household setting. The spectrum of electrical injury is very broad, ranging from minimal injury to severe multiorgan involvement, with both occult and delayed complications, to death.
Approximately 1000 deaths per year are due to electrical injuries in the United States, with a mortality rate of 3-5%.1 Classifications of electrical injuries generally focus on the power source (lightning or electrical), voltage (high or low voltage), and type of current (alternating or direct), each of which is associated with certain injury patterns.
This article reviews the pathophysiology, diagnosis, and treatment of electrical injuries caused by manufactured electricity; for further information on lightning injuries, please see Lightning Injuries.
Pathophysiology
Electricity is generated by the flow of electrons across a potential gradient from high to low concentration through a conductive material. The voltage (V) represents the magnitude of this potential difference and is usually determined by the electrical source. The type and extent of an electrical injury is determined by voltage, current strength, resistance to flow, the duration of contact with the source, the pathway of flow, and the type of current (ie, direct or alternating).
Voltage
Electrical injuries are typically divided into high-voltage and low-voltage injuries, using 500V or 1000V as the cutoff. High morbidity and mortality has been described in 600V direct current injury associated with railroad “third rail” contact.2 In the United States and Canada, typical household electricity provides 110V for general use and 240V for high-powered appliances, while industrial electrical and high-tension power lines can have more than 100,000V.3 Voltage is directly proportional to current and indirectly proportional to resistance, as expressed by Ohm’s Law:
V = I X R; where I = current, V = voltage, R = resistance.
Current
The volume of electrons flowing across the potential gradient is the current, which is measured in amperes (I). It is a measure of the amount of energy that flows through a body–energy is perceptible to the touch at a current as low as 1 mA. A narrow range exists between perceptible current and the “let go” current–the maximum current at which a person can grasp the current and then release it before muscle tetany makes letting go impossible. The “let go” current for the average child is 3-5 mA; this is well below the 15-30 A of common household circuit breakers. For adults, the “let go” current is 6-9 mA, slightly higher for men than for women. Skeletal muscle tetany occurs at 16-20 mA. Ventricular fibrillation can occur at currents of 50-100 mA.4
Resistance
The impedance to flow of electrons across the gradient is the resistance (R) and varies depending on the electrolyte and water content of the body tissue through which electricity is being conducted. Blood vessels, muscles, and nerves have high electrolyte and water content, and thus low resistance, and are good conductors of electricity–better than bone, fat, and skin.5 Heavily calloused areas of skin are excellent resistors, whereas a moderate amount of water or sweat on the skin surface can decrease its resistance significantly.
Type of circuit
Electrical current can flow in 1 of 2 types of circuits: direct current (DC) or alternating current (AC), in which the flow of electrons changes direction in rhythmic fashion. AC is the most common type of electricity in homes and offices, standardized to a frequency of 60 cycles/sec (Hz).
High-voltage DC often causes a large single muscle contraction that throws the victim away from the source; thus, usually only brief duration of contact occurs with the source flow. In contrast, AC of the same voltage is considered to be approximately 3 times more dangerous than DC, because the cyclic flow of electrons causes muscle tetany that tends to prolong victims’ exposure to the source. Muscle tetany occurs when fibers are stimulated at 40-110 Hz; thus, the standard 60 Hz of household current is within that range. If the source contact point is the hand, when tetanic muscle contraction occurs the extremity flexors contract, causing the victim to grasp the current and bring it closer to the body causing prolonged contact with the source
Types of electrical burns
Depending on the voltage, current, pathway, duration of contact, and type of circuit, electrical burns can cause a variety of injuries through several different mechanisms.
Direct contact: Current passing directly through the body will heat the tissue causing electrothermal burns, both to the surface of the skin as well as deeper tissues, depending on their resistance. It will typically cause damage at the source contact point and the ground contact point.
- Electrical arcs: Current sparks are formed between objects of different electric potential that are not in direct contact with each other, most often a highly charged source and a ground. The temperature of an electrical arc can reach 2500-5000o C, resulting in deep thermal burns where it contacts the skin. These are high-voltage injuries that may cause both thermal and flame burns in addition to injury from direct current along the arc pathway.
- Flame: Ignition of clothing causes direct burns from flames. Both electrothermal and arcing currents can ignite clothing.
- Flash: When heat from a nearby electrical arc causes thermal burns but current does not actually enter the body, the result is a flash burn. Flash burns may cover a large surface area of the body but are usually only partial thickness.
History
Electrical injuries can present with a variety of problems, including cardiac or respiratory arrest, coma, blunt trauma, and severe burns of several types. It is important to establish the type of exposure (high or low voltage), duration of contact, and falls or other trauma.
- Low-voltage AC injury without loss of consciousness and/or arrest: These injuries are <1000V exposures usually in the home or office setting. Typically, children with electrical injuries present after biting or chewing on an electrical cord and suffer oral burns. Adults working on home appliances or electrical circuits can also experience these electrical injuries. Low-voltage AC may result in significant injury if there is prolonged, tetanic muscle contraction.
- Low-voltage AC injury with loss of consciousness and/or arrest: In respiratory arrest or ventricular fibrillation that is not witnessed, an electrical exposure may be difficult to diagnose. All unwitnessed arrests should include this possibility in the differential diagnosis. Query EMS personnel, family, and coworkers about this possibility. Inquire if a scream was heard before the patient’s collapse; this may be due to involuntary contraction of chest wall muscles from electrical current.
- High-voltage AC injury without loss of consciousness and/or arrest: Usually high-voltage injuries do not cause loss of consciousness but instead cause devastating thermal burns. In occupational exposures, details of voltage can be obtained from the local power company.
- High-voltage AC injury with loss of consciousness and/or arrest: This is an unusual presentation of high-voltage AC injuries, which do not often cause loss of consciousness. History may need to come from bystanders or EMS personnel.
- Direct current (DC) injury: These injuries typically cause a single muscle contraction that throws the victim away from the source. They are rarely associated with loss of consciousness unless there is severe head trauma, and victims can often provide their own history.
- Conducted electrical weapons (CEWs) such as tasers are weapons used by law enforcement that deliver high-voltage current that is neither true AC or DC but is most like a series of low-amplitude DC shocks.15 They can deliver 50,000 V in a 5-second pulse, with an average current of 2.1 mA.16 Though they have been temporally associated with deaths in the law enforcement setting, conducted electrical devices (CEDs) in healthy volunteers have been shown to be safe without evidence of delayed arrhythmia or cardiac damage as measured by troponin I.17,16 One study of their use in 1201 law enforcement incidents showed mostly superficial puncture wounds from the device probes, and significant injuries only from trauma subsequent to shock, not from the device itself. Of 2 deaths in custody, neither was related to CEW exposure.18 Overall significant injuries from CEW exposure are rare, and usually occur due to trauma or in conjunction with intoxication.19,20
Physical
Electrical injuries can cause multiorgan dysfunction and a variety of burns and traumatic injuries. A thorough physical examination is required to assess the full extent of injuries. Occupational injuries have a high likelihood of future litigation, and physical examination findings should be documented with photographs if possible, with the proper releases, and filed in the patient’s medical record.
Overall, low-voltage exposure tends to cause less overall morbidity than high-voltage, but it is important to ensure by accurate history that a seemingly low-voltage burn was not in fact from a high-voltage source (like a microwave, computer, or TV monitor—any device that “steps-up” voltage via a transformer). Low-voltage burns can still cause cardiac arrhythmia, seizure, and long-term complications if contact is near the chest or head.
- Cardiovascular
- Patients may present in asystole or ventricular fibrillation (VF) in addition to other arrhythmias. Sudden death due to VF is more common with low-voltage AC, whereas asystole is more often associated with high-voltage AC or DC. Ventricular fibrillation can be caused at voltages as low as 50-120 mA, which is lower than the typical household current. One series showed cardiac arrhythmias following 41% of low-voltage injuries.12
- Electricity can also cause conduction abnormalities and direct trauma to cardiac muscle fibers. Survivors of electrical shock can experience subsequent arrhythmia, usually sinus tachycardia and premature ventricular contractions (PVCs). One study identified 3 cases of delayed ventricular arrhythmias up to 12 hours after the incident.21 Other studies have shown no risk of delayed arrhythmias in patients with initially normal ECGs, both in low-voltage household exposures and after CEW exposure.22,19,23,18 Long-term cardiac complications occurring from electrical injury are rare.
- Respiratory: Chest wall muscle paralysis from tetanic contraction may cause respiratory arrest if the current pathway is over the thorax. Injury to the respiratory control center of the brain can also cause respiratory arrest. The lungs are a poor conductor of electricity and generally are not as susceptible to direct injury from current as tissues with lower resistance.
- Skin: A variety of burns and thermal injuries occurs from electricity that affect the skin and soft tissues. These are often the most severe sequelae of electrical burns after cardiac arrhythmias, which may initially appear minor despite significant deep tissue injury subsequently requiring fasciotomy or amputation. Burns are often most severe at the source and ground contact points; the source is usually the hands or the head while the ground is often in the feet. The strength and duration of contact with the source largely influence severity and extent of tissue damage. All burns should be carefully documented and, if possible, photographed.
- High-voltage electrothermal burns: Typically, these show a contact point and ground point: where the person touched the circuit and where he or she was grounded. These may produce significant damage to underlying tissue while largely sparing the surface of the skin. These burns may appear as painless, depressed areas with central necrosis and minimal bleeding. The presence of surface burns does not accurately predict the extent of possible internal injuries, as skin with high resistance will transmit energy to deeper tissues with lower resistance
Arc burns: When an arc of current passes from an object of high to low resistance, it creates a high temperature pathway that causes skin lesions at the site of contact with the source and at the ground contact point (not always the feet). These areas typically have a dry parchment center and a rim of congestion around them. There will be clues to the internal pathway taken by the arc based on the location of these surface wounds. Arcs can also cause electrothermal, flash, and flame burns, so multiple burns of varying appearance may be observed. Arcs do not occur in low-voltage injuries.
Flash burns: Flash burns are caused by heat from a nearby electrical arc that can reach upwards of 5000o C. These can pass over the surface of the body or through, depending on the path of the arc causing the flash. They may “splash” over the surface of the body, resulting in diffuse but relatively superficial partial-thickness burns. There is no internal electrical component.
- Flame burns: Flame burns are caused by ignition of clothing or nearby objects. These cause thermal burns similar to other flame burns.
- Cardiovascular
- Low-voltage burns: These behave like ordinary thermal burns and range from local erythema to full-thickness burns. These require several seconds of contact to cause skin burns, sometimes reaching current levels high enough to cause VF before causing any significant skin damage.4 Direct contact burns may occur only if the circuit through the person was prolonged for more than a few seconds.
Contact burns: Contact burns usually have a pattern from the contacted item (branding) and may appear similar to flash burns. To differentiate them, full-thickness contact burns have unburned surface hair, whereas flash burns singe the hairs, which are largely gone by the time the patient presents to the ED
- Pediatric oral burns: These are most commonly encountered in children younger than 6 years who bite or suck on a household electrical cord. A local arc of current crosses from one side of the mouth to the other. The orbicularis oris muscle may be involved, and cosmetic deformity of the lips may occur if the burn crosses the commissure. Significant edema may be noted and within 2-3 days eschar formation. Life-threatening bleeding can occur at 2-3 weeks post injury if the labial artery is exposed when the eschar falls off. Initial presentations may underestimate the extent of the ultimate injury; patients require aggressive airway management.9 These patients should be referred for early follow-up to a burn specialist, plastic surgeon, and an oral surgeon.
- Neurologic
- Most acute CNS or spinal deficits resulting from electrical injuries are due to secondary blunt trauma or burns. Often, the patient has transient confusion, amnesia, and impaired recall of events if not frank loss of consciousness. Direct effects of electrical current are most severe if the respiratory control center of the brainstem is affected resulting in respiratory arrest. Current may also cause seizure or direct spinal cord injury if there is hand-to-hand flow. Spinal cord injury can result from direct current effects or blunt trauma. Unless a patient is completely lucid with full recollection of the events, initial C-spine immobilization is indicated.
- Currents cause acute muscle tetany at relatively low currents and frequencies, like those found in most households. Muscle tetany causes victims to grasp the source, prolonging contact time, and can also paralyze respiratory muscles resulting in asphyxiation.
- Long-term neurologic complications include seizures, peripheral nerve damage, delayed spinal cord syndromes, and psychiatric problems from depression to aggressive behavior.
- Musculoskeletal: Acute injuries include fracture from blunt trauma and compartment syndrome from burns. The chest and any extremity should be examined for circumferential burn. Palpate the extremity and perform distal neurologic, vascular, and motor examination to determine if there is suspicion of a compartment syndrome. If this is the case, compartment pressure can be measured and early fasciotomy may help prevent subsequent amputation.11 If available, surgical consultation should be obtained early for a patient with these concerns or for appropriate trauma consultation. Massive muscle damage can cause severe rhabdomyolysis and subsequent renal failure.
- ENT/head: The head is a common point of entry for high-voltage injuries. Patients may have perforated tympanic membranes, facial burn, and cervical spine injury. Approximately 6% of victims develop cataracts, usually months after the initial injury, with increasing frequency the closer contact is to the head.24,10
Causes
Electrical injury occurs when a person becomes part of an electrical circuit or is affected by the thermal effects of a nearby electrical arc. Injuries are caused by high-voltage AC, low-voltage AC, or DC.
- High-voltage AC: High-voltage injuries most commonly occur from a conductive object touching an overhead high-voltage power line. In the United States, most electric power is distributed and transmitted by bare aluminum or copper conductors, which are insulated by air. If the air is breached by a conductor, (eg, an aluminum pole, antenna, sailboat mast, crane), any person touching the conductor can be injured. Occupational injuries may include direct contact with electrical switching equipment and energized components.
- Low-voltage AC: Generally, 2 types of low-voltage injury occur: children biting into electrical cords producing severe lip, face, and tongue injuries, or the adult who becomes grounded while touching an appliance or other object that is energized. The latter type of injury is decreasing with the increasing use of ground fault circuit interrupters (GFCIs) in circuits where people might easily become grounded. GFCIs stop current flow in the event of a leakage current (ground fault) if the ground fault is greater than 0.005 amps (0.6 W at 120 V).
- Direct current (DC): DC injuries are generally encountered when the third energized rail of an electrical train system is contacted while the person is grounded. This sets up a circuit of electric current through the victim, causing severe electrothermal burns and myonecrosis.2
Prehospital Care
First, rescuers should practice awareness of scene safety and be sure there is no imminent threat to bystanders or responders in attempting to remove the victim from the electrical source. For high-voltage incidents, the source voltage should ideally be turned off before rescue workers enter the scene.
After ensuring scene safety, rescuers should approach victims of electrical injuries as both trauma and cardiac patients. Patients may need basic or advanced cardiac life support. They should be C-spine immobilized prior to movement, and spine immobilization as indicated by the mechanism of injury.
Given that injuries may be limited to a ventricular arrhythmia or respiratory muscle paralysis, aggressive and prolonged CPR should be initiated in the field for all electrical injury victims, as they are likely to be younger with fewer comorbid conditions and have better chances of survival after prolonged CPR.
Emergency Department Care
Stabilize patients and provide airway and circulatory support as indicated by ACLS/ATLS protocols. Obtain airway protection and provide oxygen for any patient with severe hypoxia, facial/oral burns, loss of consciousness/inability to protect airway, or respiratory distress. Full cervical spine immobilization +/- spinal immobilization as needed based on mechanism of injury. Primary survey should assess for traumatic injuries such as pneumothorax, peritonitis, or pelvic fractures.
After primary assessment, begin fluid resuscitation and titrate to urine output of 0.5-1 mL/kg/h in any patient with significant burns or myoglobinuria. Consider furosemide or mannitol for further diuresis of myoglobin. Urine alkalinization increases the rate of myoglobin clearance and can be achieved using sodium bicarbonate titrated to a serum pH of 7.5. Obtain adequate intravenous access for fluid resuscitation, whether peripheral or central. Initiate cardiac monitoring for all patients with anything more than trivial low-voltage exposures.
Burn care should include tetanus immunization as indicated, wound care, measurement of compartment pressures as indicated, and it may include early fasciotomy. Extremities with severe burns should be splinted in a functional position after careful documentation of full neurovascular examination.
The risks of electrical injury to the fetus in a pregnant patient are unknown. Pregnant women who are involved in electrical injuries should have a careful examination for traumatic injuries and obstetrical consultation. Women in the second half of pregnancy should be admitted for fetal monitoring in any cases of severe electrical injuries, high-voltage exposures, or minor electrical injuries with significant trauma.
Consultations
Patients with high-voltage electrical injuries require the ongoing care of a burn specialist, which should be instituted as early as possible, as aggressive early intervention via fasciotomy can prevent subsequent limb amputation.
Consider additional consultations with trauma/critical care, orthopedics, plastic surgery, and general surgery, depending on the type and severity of traumatic injuries.
Medication
Hydration is the key to reducing the morbidity of severe burns. If there is significant muscle damage with myoglobinuria, an osmotic diuretic and/or alkalinizing agent is indicated.
Fluids
Extravascular pooling of fluids through damaged endothelium leads to vascular hypovolemia and hypotension. Patients require fluid resuscitation with normal saline or lactated ringer.
Lactated Ringer
Essentially isotonic and has volume restorative properties.
Adult
10 mL/kg/h IV during initial resuscitation
Pediatric
Administer as in adults
None reported
Major complication of isotonic fluid resuscitation is interstitial edema; edema of extremities is unsightly but not a significant complication; edema in brain or lungs is potentially fatal; major contraindication to isotonic fluid resuscitation is pulmonary edema; added fluid promotes more edema and may lead to development of ARDS
Pregnancy
C – Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Isotonic fluids administered during resuscitation of electrical shock require close monitoring of cardiovascular and pulmonary function; stop fluids when desired hemodynamic response is observed or pulmonary edema develops
Osmotic diuretics
Osmotic diuretics assist the kidneys in excreting myoglobin if present. They can help avoid acute renal failure in patients with significant myoglobinuria.
Mannitol (Osmitrol)
Osmotic diuretic that is not metabolized significantly and that passes through glomerulus without being reabsorbed by the kidney.
Adult
50-200 g/24 h IV; adjust dose to maintain a urinary output of 30-50 mL/h
Pediatric
<12 years: Not established
Trial doses of 0.2 g/kg IV followed by careful monitoring of urinary output may be prudent; again, with the goal of producing diuresis in the child with myoglobinuria
None reported
Documented hypersensitivity; anuria; severe pulmonary congestion; progressive renal damage; severe dehydration; active intracranial bleeding; progressive heart failure
Pregnancy
C – Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Carefully evaluate cardiovascular status before rapid administration of mannitol because a sudden increase in intracellular fluid may lead to fulminating CHF; avoid pseudoagglutination; when blood administered simultaneously, add at least 20 mEq of sodium chloride to each liter of mannitol solution; do not administer electrolyte-free mannitol solutions with blood
Loop diuretics
These agents decrease plasma volume and edema by causing diuresis.
Furosemide (Lasix)
Proposed mechanisms for furosemide in lowering intracranial pressure include (1) lowering cerebral sodium uptake, (2) affecting water transport into astroglial cells by inhibiting cellular membrane cation-chloride pump, and (3) decreasing CSF production by inhibiting carbonic anhydrase.
Dose must be individualized to patient.
- Dosing
- Interactions
- Contraindications
- Precautions
Adult
Initial dosage: 20-40 mg IV slowly
Adjust dosage to maintain urinary output at 30-50 mL/h