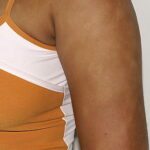
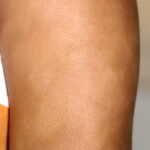
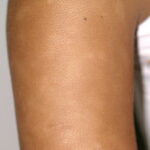
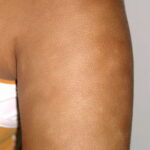
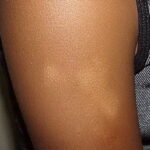
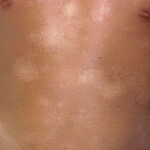
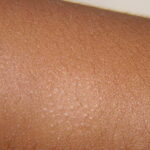
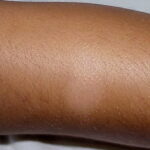
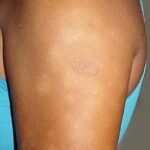
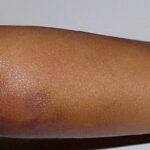
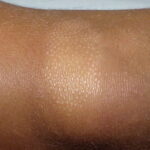
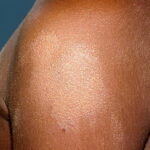
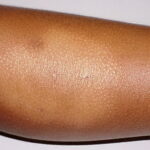
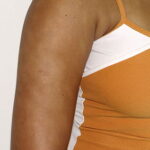
Pityriasis alba
Pityriasis alba is a term derived from the words scaly (pityriasis) and white (alba).
Debate exists as to the term extensive pityriasis alba (EPA), which some believe to be a confusing misnomer applied to a pathoetiologically different entity and has the proposed name of “progressive extensive hypomelanosis”. EPA is believed to be a primary, acquired hypopigmentation observed in females aged 18-25 years of mixed ethnic origin; it is characterized by hypochromic, nonscaly macules developing on the back and abdomen, increasing in number and progressively coalescing over the whole trunk into larger patches surrounded by smaller well-defined macules. Although the single skin lesions of EPA do not differ substantially from those of pityriasis alba, consistent differences are as follows:1
- A widespread and symmetric involvement of the trunk by numerous, round, nonscaly hypomelanotic patches without a preceding inflammatory phase and chronic in duration (This is as opposed to face predominance in pityriasis alba.)
- Histologic examination shows a decrease of epidermal melanin; spongiosis is absent.
- Ultrastructural studies suggested reduced number of active melanocytes and a decrease in number and size of melanosomes.
- No atopy and no associated pathologies or familial occurrences have been reported.
- The age of occurrence; the sex ratio (female preponderance)
- Widespread lesions of classical pityriasis alba can be observed in atopic dermatitis, but they should not be confused with the disorder described by Zaynoun as EPA.
Some authors believe EPA overlaps with another condition described “progressive and extensive hypomelanosis” in persons of mixed racial background and also reported as “progressive and confluent hypomelanosis of the melanodermic metis” or “creole dyschromia”. The alternate name of “progressive extensive hypomelanosis” has been proposed.1
Pathophysiology
No known cause of pityriasis alba has been reported. Atopy and postinflammatory changes are leading current theories as to the origin of the lesions. Theories of origin include hypopigmentation secondary to pityriacitrin, a substance produced by Malassezia yeasts, that acts as a natural sunscreen.
A large number of patients with pityriasis alba have a history of atopic disease. In addition, atopic patients are more prone to developing pityriasis alba.2
Histology of biopsy studies show features including hyperkeratosis (33.33%), parakeratosis (40%), acanthosis (53.33%), spongiosis (80%), and perivascular infiltrate (100%).2 However, these findings are not specific enough to make the diagnosis.
Atrophic sebaceous glands were noted in almost half the cases in one study.3
Anemia has been reported in up to 16% of patients.2 This may be a coincidental finding, and the clinical relevance of anemia is not yet known.
Ultrastructure studies note that despite a reduced pigment in lesional skin, there is no difference in melanocytes between lesional and nonlesional skin in the same patient, although this finding is still under debate. Degenerative changes in melanocytes and reduced keratonocyte melanosomes were also noted.3 Overall, the defect is believed to be due to decreased melanin
History
- Pityriasis alba lesions often occur on the face. In particular, the cheek is a common site.2
- Lesions may be erythematous or pruritic in the beginning, evolving into scaly, hypopigmented macules. Patients may complain that lesions are more prominent in the summer, secondary to the surrounding hyperpigmentations associated with prolonged sun exposure.
Physical
- A flaky, hypopigmented, patchy dermatitis with fine scales involving the face and, at times, the neck and shoulders typically is found.
- Numerous (up to 20 or more) hypopigmented macules, which are ill defined and range in size from 1-4 cm, can be found
- The lesions of pityriasis alba tend to have less well-defined borders than lesions seen in vitiligo, and they do not coalesce as seen in tinea versicolor.
- An association with atopy is believed to exist; therefore, some patients may have atopic dermatitis as well.
- Other clues of atopic changes can help and also distinguish atopic from atopiform patients. These include Dennie-Morgan folds, perioral pallor, and a horizontal nasal crease on the root of the nose. In particular, a history of atopy, recurrent conjunctivitis, palmar hyperlinearity, keratosis pilaris, pityriasis alba, and hand and/or food eczema were significantly less present in atopiform dermatitis. Dennie-Morgan fold was positively associated with atopiform dermatitis.4
Causes
No definitive etiologic agent has been described for pityriasis alba.
Other Problems to Be Considered
Mycosis fungoides: This is of particular concern for lesions that are atypical in any way. This includes lesions that are persistent, symptomatic, or changing in color or shape.
Leprosy: This condition also is critical to diagnose. This must be considered in arid regions, including areas with armadillo exposure in the United States. In particular, association with the 7 banded armadillo in the southern United States has been described.
Delusional tinea: Delusional disorders may result in chronic postinflammatory hypopigmentation changes. It may be possible for such a lesion to appear like pityriasis alba.
Nevus depigmentosa: This tends to occur on the trunk, is segmental in distribution, and does not change in size or number over time.
Workup
Laboratory Studies
- A workup may be undertaken to exclude other causes of hypopigmentation; however, most of this would be accomplished through a dermatology referral.
- As an emergency physician, a Wood’s light examination may help in evaluating the patient whose rash is due to vitiligo. Vitiligo will glow more brightly and will have edges with sharper demarcation.
- Potassium hydroxide stain of a skin scraping will be positive if the patient has tinea versicolor, which has an alternate name of pityriasis versicolor. This would likely be performed by a dermatologist.
- A biopsy would be required for atypical lesions as noted in the differential. This would likely be performed by a dermatologist.
Other Tests
- Hypopigmentation may occur in other disorders, such as those caused by fungi (eg, tinea versicolor), previous inflammatory conditions (eg, postinflammatory hypopigmentation), idiopathic disorders (eg, vitiligo), or malignancy (mycosis fungoides), or it may occur secondary to medications such as retinoic acid, benzoyl peroxide, and topical steroids. Clinicians should rule out these other disorders when evaluating a patient who may have pityriasis alba.
Procedures
- A biopsy of the lesions usually is not necessary and is not indicated in the emergency department. Pathologic findings are nonspecific; however, findings may include a basal layer with irregular pigmentation, follicular plugging, edema between epithelial cells (ie, spongiosis), or atopy of the sebaceous glands. However, this is required in atypical cases and should be performed in the office of a specialist in skin disease. It is of particular concern, considering the common location of the cheek and the potential approximation of this area to the facial artery.
- Details of biopsy results are noted in Pathophysiology.
Medication
Because the disease usually is self-limited and asymptomatic, medical therapy is often unnecessary. Pityriasis alba has no medical consequences, and the side effects of the medications may outweigh the cosmetic benefit of intervention. The most commonly used remedies (eg, emollients, topical steroids, psoralen plus ultraviolet light A photochemotherapy [PUVA]) appear to have limited efficacy.
Emollients are used to reduce the scaling of the lesions, especially on the face.
Topical steroids may help with erythema and pruritus during the initial lesions and may accelerate repigmentation of existing lesions. Use should be limited, with frequent breaks from use, to avoid long-term skin atrophy and steroid changes.
Psoralen plus ultraviolet light A photochemotherapy (PUVA) may be used to help with repigmentation in extensive cases, although the recurrence rate is high after treatment is stopped.
Pimecrolimus 1% has also been proposed as an option over a 3-month period.5
Corticosteroids, topical
These agents have anti-inflammatory properties and cause profound and varied metabolic effects. They modify the body’s immune response to diverse stimuli.
Hydrocortisone topical (Cortaid, Cortizone-10)
An adrenocorticosteroid derivative suitable for application to skin or external mucous membranes. Has mineralocorticoid and glucocorticoid effects, resulting in anti-inflammatory activity.
Adult
Apply sparingly to affected areas bid/qid
Pediatric
Apply as in adults