dermatophytes
The dermatophytes are a group of fungi (ringworm) that invade the dead keratin of skin, hair, and nails. Several species of dermatophytes infect humans; these can be divided into superficial and deep forms. This article focuses on superficial fungal infections that mainly belong to the Epidermophyton, Microsporum, and Trichophyton genera. These are more common and more likely to be seen in the ED. More detailed information can be found in the Dermatology section on deep fungal infections that can be life threatening in presentation, most often present in those with little or no immune response ability, and require immediate dermatologic consultation.
Dermatophytosis is a superficial fungal infection caused by dermatophytes. The infection may spread from person to person (anthropophilic), animal to person (zoophilic), or soil to person (geophilic). The most common of these organisms are Trichophyton rubrum, Trichophyton tonsurans, Trichophyton interdigitale and/or Trichophyton mentagrophytes, Microsporum canis, and Epidermophyton floccosum.
The term phyton is derived from the Latin/Greek word for plant. Thus, dermato (skin) phyte (plant) was generated as a descriptive early term for tinea on the skin.
The term tinea is derived from the Latin word for worm or larvae.
Pathophysiology
Dermatophytes are keratinophilic fungi and have the ability to invade keratinized tissue (eg, hair, nails, any area of the skin) but are restricted to the dead cornified layer of the epidermis. Humid or moist skin provides a very favorable environment for the establishment of fungal infection. Clinically, tinea infections are classified according to the body region involved/infected:
Tinea corporis – Trunk and extremities
- Tinea manuum and tinea pedis – Palms, soles, and interdigital webs
- Tinea cruris – Groin
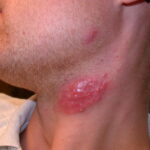
- Tinea barbae – Beard area and neck
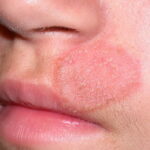
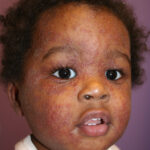
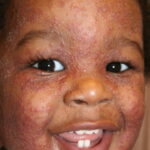
- Tinea faciale – Face
- Tinea unguium (onychomycosis) – Nail
Descriptive clinical diagnoses also exist and are based on old derivations of terminology. One example is tinea imbricata, which forms geometric patterns on the skin.1
The specific etiologic agent is often associated with a specific region of infection. Further elaboration of the discussion below can be found in the tinea articles of the eMedicine Dermatology volume (Tinea Barbae, Tinea Capitis, Tinea Corporis, Tinea Cruris, Tinea Faciei, Tinea Nigra, Tinea Pedis, Tinea Versicolor).
Tinea capitis caused by the species of genera Trichophyton and Microsporum) is the most common pediatric dermatophyte infection. The age predilection is believed to result from the lack of certain flora and fungistatic sebum in this age (Pityrosporum orbiculare [Pityrosporum ovale]) and short/medium chain fatty acids.)
From the site of inoculation, the fungal hyphae grow centrifugally in the stratum corneum and down into the hair as they invade newly forming keratin. It usually takes 2 weeks to produce clinically visible changes.
The natural course of tinea capitis is of a spontaneous cure at puberty, once sebum production begins.
Hair invasion is divided into 3 types. The site of formation of the arthroconidia (spore-forming bodies) classifies the species causing the invasion. They are as follows:- Ectothrix species: Conidia form on the exterior of the hair shaft. The cuticle is destroyed and involved areas fluoresce a green-yellow under a Wood lamp. This is caused by Microsporum canis, Microsporum distortum, Microsporum ferrugineum, Microsporum audouinii, as well as nonfluorescent Trichophyton rubrum,Trichophyton verrucosum, Trichophyton megninii, Trichophyton mentagrophytes, Microsporum gypseum, and Microsporum nanum.
- Endothrix species: Conidia form within the hair shaft, and each is filled with hyphae and spores. The cuticle is not affected, and hairs do not fluoresce under a Wood lamp. This is caused by anthropophilic (Trichophyton rubrum, Trichophyton gourvilii, Trichophyton tonsurans,Trichophytonviolaceum,Trichophyton yaoundei, Trichophyton soudanense).
- Favus species: Hyphae arrange within and around the hair shaft. This is a rare and severe form resulting in favus-like crusts or scutula and hair loss with honey comb destruction pattern of the follicles. This is caused by Trichophyton schoenleinii.
- Kerion: Thick plaques and boggy skin that form often with bacterial infection superimposed. Mainly caused by Microsporum canis.2 This pattern develops in such a manner that it is often believed to be a response to the dermatophyte.
History
- It takes about 2 weeks from inoculation to subsequent skin changes that are clinically visible.
- Pruritus (itching) is the main symptom in most forms of tinea. Findings can be subtle and care must be taken in examination, as a novel form of delusional tinea has been described in several reports.6
- Patients with tinea capitis have hair loss. Infected hairs are brittle and break easily.
- Asking the patient about participation in sports, such as judo, karate, wrestling, and other contact sports, is important. Likewise, asking the patient about military enrollment and any contacts with similar skin disease is important.
Physical
At physical examination, the various types of tinea may have different findings, as follows:
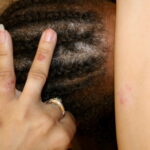
- Tinea capitis
- The clinical appearance of fungal infection of the scalp varies depending on the type of hair invasion.
- Alopecia (hair loss), with hairs breaking at the scalp surface, usually is present.
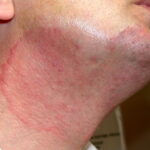
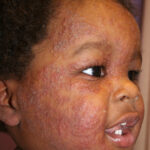
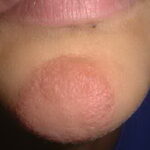
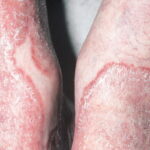
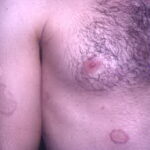
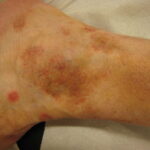
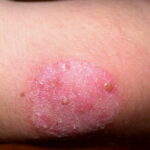
- Tinea corporis
- Infection typically is on the exposed skin of the trunk and extremities.
- It is characterized by annular scaly plaques with raised edges, pustules, and vesicles. It can also have geometric patterns. This is usually tinea imbricata (Trichophyton concentricum).
- Tinea corporis gladiatorum is seen on the head, neck, and arms, in a distribution consistent with the areas of skin-to-skin contact in wrestling.
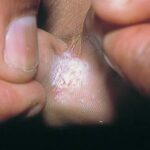
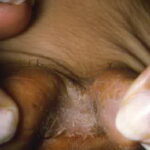
- Tinea pedis
- This is a fungal infection of the toe webs and plantar surface and often affects only one foot.
- Toe-web scaling, fissuring, and maceration; scaling of soles and lateral surfaces; erythema; vesicles; pustules; and bullae may be present.
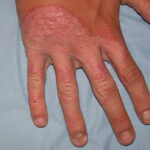
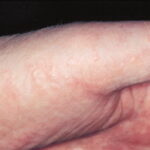
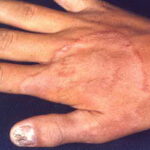
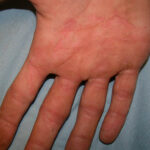
- Tinea manuum
- This is a fungal infection of the palms and finger webs that usually occurs in association with tinea pedis.
- Usually, only one hand is involved.
- Scaling and erythema may be present.
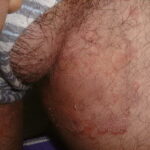
- Tinea cruris
- It is a dermatophytic infection of the groin and pubic region.
- It is characterized by erythematous lesions with central clearing and raised borders.
- Tinea cruris often co-occurs with tinea pedis or tinea unguium.
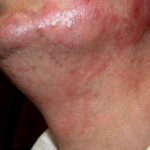
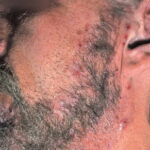
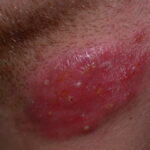
- Tinea barbae
- The beard and neck area are affected.
- Erythema, scaling, and pustules are present.
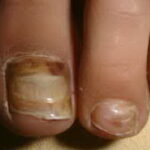
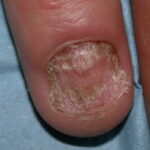
- Tinea unguium
- Tinea unguium is also called onychomycosis; this is an infection of the nail.
- It is characterized by onycholysis (nail plate separation from nail bed) and thickened, discolored (white, yellow, brown, black), broken, and dystrophic nails.
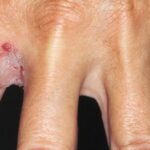
- Majocchi granuloma
- This is a deep folliculitis-like infection.
- Majocchi granuloma is kerionlike, characterized by erythema and nodules.7
- Treatment may require a slightly higher dose; this infection is more chronic in nature than typical tinea hair-related infections.
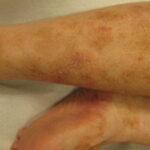
- Id reaction (ie, identity reaction)
- Id reaction is a fungus-free eruption that can resemble tinea.
- Is secondary to a tinea infection at another site, is due to cell-mediated immunity, and resolves with treatment of tinea.
- Tinea imbricata as noted above.
- Tinea incognito: This is a common difficult diagnosis to make without history. It is often present as a result of prior treatment with hydrocortisone causing atypical appearance.8
Causes
The various tinea infections are caused chiefly by species of the genera Microsporum, Trichophyton, and Epidermophyton.
Tinea corporis is mainly caused by T tonsurans and also by M canis and T rubrum.
Risk factors for tinea infection include the following:- Moist conditions
- Communal baths
- Immunocompromised states
- Cushing syndrome
- Atopy
- Genetic predisposition
- Athletic activity that causes skin tears, abrasions, or trauma such as wrestling, judo, or soccer
Laboratory Studies
- Direct microscopic examination may be performed.
- Skin scrapings, nail specimens, or plucked hairs are treated with potassium hydroxide and examined.
- Hyphae can be visualized in skin and nails.
- Spores within or around the hair shaft can be detected.
- Fungal cultures can be performed for precise identification of the species.
- Wood light (UV light) examination may be performed.
- This examination is used mainly for the diagnosis of tinea capitis.
- Hairs infected with Microsporum audouinii and M canis produce a brilliant yellow-green fluorescence. This is detailed in the Pathophysiology section above.
- Trichophyton schoenleinii causes a dull green fluorescence.
- Histology is not needed, but biopsy findings would show spongiosis, parakeratosis (that may alter with orthokeratosis), and a superficial inflammatory infiltrate. Neutrophils may be seen in the stratum corneum, which is a significant diagnostic clue. On occasion, septate branching hyphae are seen in the stratum corneum. Special fungal stains (eg, periodic acid-Schiff, Gomori methenamine silver) may be required.
Medication
Tinea corporis infections may be treated with topical agents (ie, creams, lotions, solutions, powders, sprays) as the drug of choiceor with oral antifungals in extensive or recalcitrant disease.10,11
For tinea capitis and nail infections, topical therapy is ineffective. Findings with onychomycosis treatment were discouraging because of the need for prolonged therapy and the low success rate. However, in recent years, new oral antimycotic drugs have been developed as the drug of choice; these have greatly improved the outlook (especially for patients with fungal toenail infection).12
Use of oral medications requires baseline LFT checks as well as repeat labs half way through the typical 3 month course. Cultures are also recommended when managing children, as oral medications are more difficult for this age group.13
Medication classes- Two classes of antifungal medications are most commonly used: azoles and the allylamines.
- Both classes have the common endpointoif inhibiting ergosterol production.
- Azoles inhibit lanosterol 14-alpha-demethylase, an enzyme that converts lanosterol to ergosterol (important for the fungal cell wall). This leads to permeability and renders the fungus unable to reproduce.
- Allylamines inhibit squalene epoxidase, an enzyme that converts squalene to ergosterol, leading to the accumulation of toxic levels of squalene in the cell and cell death.
Antifungals
The optimal duration of topical therapy for dermatophytic infections of the skin has never been established. In most cases of tinea corporis and tinea cruris, 2 weeks of treatment may suffice. Tinea pedis may require treatment for as long as 8 weeks.
Ketoconazole 2% cream (Nizoral)
Imidazole, broad-spectrum antifungal agent indicated for the topical treatment of tinea corporis, tinea cruris, and tinea pedis. Inhibits synthesis of ergosterol (main sterol of fungal cell membranes), causing cellular components to leak; results is cell death.
Adult
Rub gently into affected area qd or bid for 2-4 wk
Pediatric
Administer as in adults
None reported
Documented hypersensitivity
Pregnancy
C – Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
If sensitivity or irritation develops, discontinue use; for external use only; avoid contact with eyes
Clotrimazole 1% cream or lotion (Lotrimin, Mycelex)
Indicated for topical treatment of tinea corporis, tinea cruris, and tinea pedis. Broad-spectrum antifungal agent that inhibits yeast growth by altering cell membrane permeability, causing fungal cell death.
Adult
Gently massage into affected and surrounding skin areas bid for 2-6 wk
Pediatric
Administer as in adults
None reported
Documented hypersensitivity
Pregnancy
B – Fetal risk not confirmed in studies in humans but has been shown in some studies in animals
Precautions
If sensitivity or chemical irritation occurs, discontinue use; use only externally; avoid contact with eyes
Econazole 1% cream or lotion (Spectazole)
Effective in cutaneous infections. Interferes with RNA and protein synthesis and metabolism. Disrupts fungal cell-wall membrane permeability, causing fungal cell death.
Adult
Apply sparingly over affected areas qd for 2-6 wk
Pediatric
Administer as in adults
None reported
Documented hypersensitivity
Pregnancy
C – Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
If sensitivity or irritation develops, discontinue use; for external use only; avoid contact with eyes
Miconazole 2% cream (Monistat, Daktarin)
Damages fungal cell-wall membrane by inhibiting biosynthesis of ergosterol. Membrane permeability is increased, causing nutrients to leak and resulting in fungal-cell death. The lotion is preferred in intertriginous areas. If the cream is used, apply sparingly to avoid maceration effects.
Adult
Cream and lotion: Cover affected areas bid for 2-6 wk
Powder: Spray or sprinkle liberally over affected area bidPediatric
Administer as in adults
None reported
Documented hypersensitivity
Pregnancy
C – Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
If sensitivity or chemical irritation occurs, discontinue use; use only externally; avoid contact with eyes
Terbinafine (Lamisil)
Synthetic allylamine derivative that inhibits squalene epoxidase, a key enzyme in sterol biosynthesis of fungi, resulting in a deficiency in ergosterol that causes fungal cell death. Use until symptoms significantly improve.
Adult
Terbinafine tab
Tinea cruris, tinea corporis: 250 mg/d PO for 2-4 wk
Tinea pedis: 250 mg/d PO for 2-6 wk
Tinea capitis: 250 mg/d PO for 4 wk
Fingernail infection: 250 mg/d PO for 6-8 wk
Toenail infection: 250 mg/d PO for 3-4 mo
Terbinafine 1% cream
Tinea corporis, tinea cruris: Apply to affected area qd for 1-4 wk
Tinea pedis: Apply to affected area bid for 1-4 wkPediatric
Terbinafine tab, treatment duration similar to that in adults
12-20 kg: 62.5 mg/d PO
20-40 kg: 125 mg/d PO
>40 kg: 250 mg/d PO
Terbinafine 1% cream
<12 years: Not established
>12 years: Administer as in adults Coadministration of PO form may increase cyclosporine clearance; rifampin and phenobarbital may decrease terbinafine level; cimetidine may decrease terbinafine clearance
Documented hypersensitivity
Pregnancy
B – Fetal risk not confirmed in studies in humans but has been shown in some studies in animals
Precautions
Discontinue use if chemical irritation or signs of hepatobiliary dysfunction develop; topical dosage form is for external use only; avoid contact with eyes
Naftifine 1% cream (Naftin)
Indicated for the treatment of tinea corporis, tinea cruris, and tinea pedis. Broad-spectrum antifungal agent that appears to interfere with sterol biosynthesis by inhibiting the enzyme squalene 2,3-epoxidase. This inhibition results in decreased amounts of sterols, causing cell death. If no clinical improvement occurs after 4 weeks of treatment, reevaluate the patient.
Adult
Cream: Gently massage sufficient quantity into affected area and surrounding skin qd for 2-4 wk
Gel: Gently massage sufficient quantity into affected and surrounding skin areas bid for 2-4 wkPediatric
Administer as in adults
None reported
Documented hypersensitivity
Pregnancy
B – Fetal risk not confirmed in studies in humans but has been shown in some studies in animals
Precautions
Discontinue use if sensitivity or chemical irritation occurs; for external use only; avoid contact with eyes
Griseofulvin (Gris-PEG, Grifulvin V, Fulvicin, Griseofulvin)
Extensively used in the past to treat dermatophytic infections of the skin. However, with new antifungals now available, use is now limited. An antibiotic derived from a species of Penicillium that is deposited in the keratin precursor cells, which are gradually replaced by noninfected tissue; the new keratin then becomes highly resistant to fungal invasions. Most used therapy for treating tinea capitis, especially if caused by M canis.
Adult
Tinea corporis, tinea cruris, and tinea capitis: 500 mg microsize (330-375 mg ultramicrosize) PO in single or divided daily doses for 2-6 wk
Tinea pedis, tinea unguium: 0.75-1 g microsize (660-750 mg ultramicrosize) PO in single or divided doses for 2-6 wkPediatric
11 mg microsize/kg/d (5 mg/lb/d) PO or 7.3 mg ultramicrosize/kg/d (3.3 mg/lb/d) PO
May decrease hypoprothrombinemic activity of warfarin; patients may require a dosage adjustment; oral contraceptives may lose effectiveness when administered concurrently, possibly leading to breakthrough bleeding, amenorrhea, or unintended pregnancy; may reduce effects of cyclosporine; may decrease serum salicylate concentrations; barbiturates may decrease serum levels
Documented hypersensitivity
Pregnancy
C – Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
For prolonged therapy, observe patients closely; monitor renal, hepatic, and hematopoietic function regularly; lupuslike syndromes or exacerbation of lupus erythematosus may occur; photosensitivity may occur; patients should take protective measures against exposure to UV light or sunlight
Itraconazole (Sporanox)
Synthetic triazole antifungal agent that inhibits fungal cell growth by inhibiting the cytochrome P-450–dependent synthesis of ergosterol, a vital component of fungal cell membranes.
A 30-d course of 100 mg of itraconazole daily has been shown to effectively treat tinea capitis. This treatment could prove to be a beneficial alternative to griseofulvin therapy.Adult
Tinea corporis, tinea cruris: 100 mg/d PO 2 wk or 200 mg/d PO for 1 wk
Tinea pedis: 200 mg bid PO for 1 wk
Toenail infection: 200 mg bid PO 1 for wk, given 1 wk/mo for 3-4 mo
Fingernail infection: 200 mg PO bid for 1 wk, given 1 wk/mo for 1-2 mo
Tinea capitis: 5 mg/kg/d (max dose 100 mg/d) PO for 2-4 wkPediatric
Not established
Suggested dose in children 3-16 years: 100 mg/d PO for 1 wkAntacids may reduce absorption; edema may occur with coadministration of calcium-channel blockers (eg, amlodipine, nifedipine); hypoglycemia may occur with sulfonylureas; may increase tacrolimus and cyclosporine plasma concentrations when high doses are used; rhabdomyolysis may occur with coadministration of HMG-CoA reductase inhibitors (lovastatin or simvastatin); coadministration with cisapride can cause cardiac rhythm abnormalities and death; may increase digoxin levels; coadministration may increase plasma levels of midazolam or triazolam; phenytoin and rifampin may reduce itraconazole levels (phenytoin metabolism may be altered)
Documented hypersensitivity
Pregnancy
C – Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Caution in hepatic insufficiencies; absorption impaired when gastric acidity is decreased; discontinue if neuropathy attributable to itraconazole occurs
Fluconazole (Diflucan)
Broad-spectrum triazole antifungal agent. A potent and selective inhibitor of fungal enzymes necessary for ergosterol synthesis. Most commonly used in the treatment of candidiasis.
Adult
Tinea corporis, tinea cruris: 150 mg/wk PO for 2-4 wk
Tinea pedis: 150 mg/wk PO for as long as 6 wk
Toenail infection: 150 mg/wk PO for 6-12 mo
Fingernail infection: 150 mg/wk PO for 3-6 moPediatric
Not established
Levels may increase with hydrochlorothiazides; levels may decrease with chronic coadministration of rifampin; coadministration may decrease phenytoin concentrations; may increase concentrations of theophylline, tolbutamide, glyburide, and glipizide; effects of anticoagulants may increase with coadministration; increases in cyclosporine concentrations may occur when administered concurrently
Documented hypersensitivity
Pregnancy
C – Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Monitor patient closely if rashes develop, and discontinue drug if lesions progress; may cause clinical hepatitis, cholestasis, and fulminant hepatic failure (including death) with underlying medical conditions such as AIDS, malignancy, or multiple concomitant medications; not recommended for breastfeeding women
Sertaconazole nitrate cream (Ertaczo)
Topical imidazole antifungal active against T rubrum, T mentagrophytes, E floccosum. Indicated for tinea pedis.
Adult
Apply topically bid to clean, dry skin between the toes and the immediate surrounding healthy skin
Pediatric
<12 years: Not established
>12 years: Administer as in adults