Coccidioidomycosis is an infection caused by the soil-inhabiting fungi Coccidioides immitis and Coccidioides posadasii. These fungi are endemic to certain regions of North and South America. The endemic areas in the United States include Arizona, south central California (San Joaquin Valley), Nevada, New Mexico, and the western half of Texas. Other endemic areas are the regions of Mexico that border the western United States. The fungi also are endemic to some Central American countries, including Guatemala, Honduras, and Nicaragua. Other areas, such as desert regions of South America (Argentina, Paraguay, Venezuela), also are endemic.
Historical perspectives
Wernicke and Posadas first described a case of coccidioidomycosis in 1892 in South America. Two years later in the United States, a patient with disseminated coccidioidomycosis was first reported in California in 1894. In 1896, Rixford and Gilchrist reported a few cases in which they identified the infecting agent as a protozoanlike organism and named it Coccidioides immitis. Ophuls further described the fungal life cycle and pathology of C immitis in 1905. The case of Harold Chope, a Stanford University medical student, is instructive. He inhaled a culture of Coccidioides in 1929 and went on to develop erythema nodosum and respiratory symptoms. The epidemiology of coccidioidomycosis was studied by Charles E. Smith in the Joaquin Valley after he and his colleagues developed coccidioidin skin test and serologic testing for coccidioidomycosis.
Two species of Coccidioides have been isolated: C immitis, geographically located and limited to the San Joaquin Valley, and C posadasii, located in all other endemic regions. Few clinical and immunologic differences are noted between the 2 species of Coccidioides. For all intents and purposes, all subsequent references to C immitis also apply to C posadasii.
The first effective therapy for coccidioidomycosis, intravenous amphotericin B, was first used in 1957. Since the 1980s, various oral antifungal agents, including ketoconazole, itraconazole, and fluconazole, have led to further advances in the treatment of coccidioidomycosis.
Life cycle of C immitis (and C posadasii)
C immitis and C posadasii are fungi that thrive in soil and exist in either of 2 phases—the mycelial arthrospore phase in the soil or the spherule endospore phase in infected tissues. These are hardy endemic fungi that can exist in the dry desert for months to years. During the rainy season, the mycelia grow rapidly, but they are also the least infectious. As the soil becomes dryer, the branching, septated hyphae develop into arthrospores, which readily disarticulate as single arthroconidia and become airborne when disturbed by wind or soil excavation. An arthrospore measures 3-5 µm, and it remains viable for long periods. Of note, the fungus does not grow at elevations higher than 3700 feet.
Once inhaled, an arthrospore develops into a thick-walled spherule filled with endospores. The spherules eventually open and release the hundreds of endospores. Each endospore leads to the development of a new spherule and further proliferation of the infection. These aspects of the life cycle provide further insight in the acquisition of infection and disease caused by Coccidioides.
Acquisition of infection
Coccidioidomycosis is not transmitted from person to person. Infection is usually confined to subjects in the endemic regions of North and South America as defined in Background, with most cases seen in the southwestern United States. A travel history is important because cases can be imported. The incidence of infection is highest in the dry summer months, extending into the late fall. The infection rate has been noted to increase following periods of increased rainfall (winter or summer), corresponding to increased mycelial growth.
Dust exposure is integral in acquiring infection. This risk is highlighted by circumstances in which more exposure to soil and dust occurs, such as with new construction, archeological excavation, and, most notably, following the Northridge, California earthquake of 1994. An increased incidence in infections has been noted over the past decade, attributable to a variety of factors. In addition to new construction, the population in the southwestern United States has also increased, increasing the number of susceptible hosts. Additionally, an increased awareness of the infection has also led to increased diagnosis. Noted that laboratory personnel can become infected when opening and inhaling microbiologic cultures growing Coccidioides; therefore, proper precautions are necessary whenever Coccidioides is suspected.
Pathophysiology
Inhalation of arthrospores is the portal of entry for the vast majority of coccidioidal infections. Once in the respiratory tract, spherules proliferate, and host cell–mediated immunity is crucial for controlling the infection. This is lymphocyte mediated (CD4+ CD8+ and CD20+), and the development of cell-mediated immunity, as measured by skin test reactivity to coccidioidin, can predict control of the infection. The lack of skin test reactivity has been associated with an increased risk of disseminated disease. Defects in antigen-presenting dendritic cells has been suggested as a possible explanation for failure of host containment.
The immune response to coccidioidal infection is used in the diagnosis and assessment of the severity of infection. Immunoglobin M (IgM) can be detected in 50% of primary coccidioidal infections within the first week and in 90% of infections by the third week. Immunoglobulin G (IgG) is used to gauge the intensity of the immune response and provides information on the host control of the infection and risk for disseminated (extrathoracic) disease. IgG may not be detected for several months, but it can persist for years. Note that most (60%) of coccidioidal infections are subclinical and never come to medical attention.
Clinical syndromes
Because the respiratory tract is the portal of entry, the manifestations of the initial infection are often detected after plain chest radiography. Findings include (1) unilateral infiltrate, (2) consolidation, (3) hilar adenopathy, (4) pleural effusion, (5) nodules, and (6) thin walled cavities. Depending on the host’s immune response, infection with C immitis may evolve into one of the clinical syndromes described below.
Primary pulmonary coccidioidomycosis/acute pneumonia
Up to 60% of patients with primary pulmonary coccidioidomycosis are asymptomatic or have subclinical disease that never comes to medical attention, and the infection resolves spontaneously. Those who become symptomatic manifest a respiratory syndrome approximately 1-3 weeks following inhalation of arthrospores. The symptoms are indistinguishable from other respiratory illnesses, with fever, sore throat, cough, headache, fatigue, and pleuritic chest pain. The symptoms are often attributed to a virus or community-acquired pneumonia. Resolution occurs over several weeks, and 95% or more of patients recover without any further sequelae.
If chest radiography is performed, common findings include segmental or lobar infiltrates, consolidation, and hilar adenopathy. In endemic regions, infiltrates and adenopathy are highly suggestive of coccidioidal pneumonia. Pleural effusions may be seen in up to 15% of patients and are exudative; pleural fluid eosinophilia is a common finding. Approximately 20% of these effusions may eventually be determined to be an empyema. In addition, cutaneous manifestations such as erythema multiforme or erythema nodosum are associated with the acute infection and predict a favorable outcome. Also see Coccidioidomycosis.
More extensive pneumonia, respiratory failure, and the acute respiratory distress syndrome can also be seen, often associated with inhalation of a large number of arthrospores or related to an underlying immunocompromised state (eg, HIV infection, immunosuppressant therapy, immune-modulating therapy).
In approximately 5% of patients, a pulmonary focus of coccidioidomycosis may persist and manifest as a nodule, cavity, or chronic progressive pneumonia. Coccidioides can also disseminate to involve extrathoracic sites, including bone, joints, skin, and meninges.
Chronic progressive coccidioidal pneumonia
Patients with symptoms that persist beyond 3 months define patients with chronic progressive coccidioidal pneumonia. Symptoms may include a low-grade fever, chronic cough, chest pain, hemoptysis, and weight loss. Cavitary lesions with associated infiltrates or fibrosis are typical findings and may resemble pulmonary tuberculosis. However, cocci serologies are uniformly positive. Persistent disease warrants extended antifungal therapy, ranging from years to life long.
Pulmonary nodules
In approximately 5-7% of patients with coccidioidal pneumonia, the infection evolves to form a sharply circumscribed, usually noncalcified, pulmonary nodule. This is often the initial finding on the chest radiograph, and nodules usually measure 1-2 cm. Serologic testing is positive in 30-60% of nodules. The nodules may cavitate or may persist for years. Malignancy is a major concern while evaluating these nodules. Fluorodeoxyglucose positron-emission tomography (FDG-PET) scanning cannot be used to distinguish between malignant and coccidioidomas in an endemic area. If a noninvasive diagnosis cannot be made, surgical resection may be required. In a review of 200 solitary pulmonary nodules surgically resected from patients within endemic areas, 33.5% were found to be malignant.1
Pulmonary cavities
Another manifestation of persistent pulmonary coccidioidomycosis is cavity formation. This occurs in approximately 5% of patients. The typical coccidioidal cavity is thin walled, solitary, and peripheral in location, but thick-walled cavities have also been reported. Coccidioidal cavities are usually asymptomatic, but they can be subject to hemorrhage, rupture (pneumothorax), and secondary infection. Cavities smaller than 2.5 cm typically resolve spontaneously over 1-2 years. However, cavities larger than 5 cm often persist and can be associated with hemoptysis, with the development of an aspergilloma or mycetoma in the cavity. In the past, these cavities often were surgically resected, but this has diminished since the advent of effective antifungal therapy.
Disseminated coccidioidomycosis (nonmeningeal and meningeal)
Disseminated coccidioidomycosis usually occurs within weeks to months of the primary pneumonia. Some patients may have no radiographic evidence of previous pulmonary disease, and no history of a preceding respiratory illness may be present. Certain ethnic groups, such as African Americans and Filipinos, are more likely to develop disseminated disease. Women in their third trimester of pregnancy and infants younger than 1 year are also at risk for dissemination. Any condition that compromises cellular immunity also increases the risk of dissemination; this includes patients with HIV infection, organ transplants, or hematologic malignancies and patients on immunosuppressant agents such as high-dose corticosteroids or tumor necrosis factor inhibitors.
Disseminated coccidioidomycosis usually results from hematogenous spread and can involve nearly any body site. Common meningeal sites include skin, soft tissue, bones, and joints. Other reported sites of involvement include the upper airway, myocardium, pericardium, liver, spleen, kidneys, prostate, male and female genital tracts, and lymph nodes. Dissemination is typically associated with complement fixation titers greater than or equal to 1:16. Often, combined medical and surgical therapy is required for disease control.
Meningeal involvement is a particularly severe form of disseminated coccidioidomycosis. Prior to effective therapy, meningeal coccidioidomycosis was uniformly fatal and, even with therapy, is associated with significant morbidity. Headache is the most common presenting symptom, and other neurologic symptoms include alterations in sensorium, cranial nerve defects, and obstructing hydrocephalus. Diagnosis requires analysis of cerebrospinal fluid, and typical findings include positive cerebrospinal fluid serology, elevated white blood cell count, elevated total protein values, and decreased glucose levels. Meningeal enhancement can be seen on computed tomography (CT) or magnetic resonance imaging (MRI) scans. Patients usually require life-long antifungal therapy.
History
Most coccidioidal infections are asymptomatic. Approximately 30-40% of individuals develop clinical symptoms after infection. The disease spectrum ranges from a mild influenzalike illness, to subacute pneumonia, to, rarely, respiratory failure.
- Most symptomatic patients have a febrile respiratory illness beginning 7-21 days after exposure (mean incubation period = 10-16 d).
- Most patients report cough, chest pain, fever, and fatigue.
- A study by Johnson and colleagues reported the following symptoms2 :
- Cough (73%)
- Chest pain (44%)
- Shortness of breath (32%)
- Fever (76%)
- Fatigue (39%)
- Chills (29%)
- Erythema nodosum (26%)
- Other symptoms include the following:
- Night sweats
- Weight loss
- Urticaria
- Arthralgias (“desert rheumatism”)
Physical
No physical findings are pathognomonic for coccidioidal infection. However, in endemic areas, coccidioidal infection should be a strong consideration for patients who present with an influenzal illness and a lower extremity rash.
Primary coccidioidal infection
- Skin
- Maculopapular lesions
- Erythema multiforme
- Erythema nodosum (good prognostic indicator for recovery from coccidioidomycosis)
- Toxic erythema
- Musculoskeletal – Nonspecific arthralgias and myalgias (often referred to as “desert rheumatism”)
- Pulmonary (most common physical findings)
- Rhonchi and wheezing with bronchitis, bronchiolitis, reactive airways disease
- Crackles, consolidative findings, decreased breath sounds and pleural friction rub associated with pneumonia and pleural effusion/empyema
- Decreased breath sounds associated with a bronchopleural fistulas and pneumothorax
Disseminated coccidioidal infection
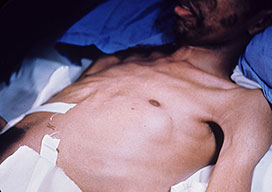
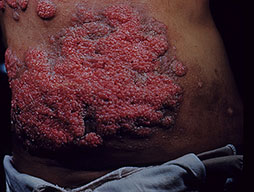
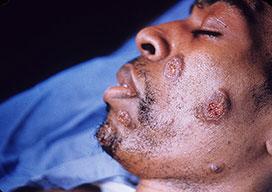
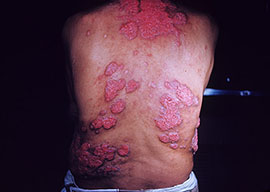
- Skin
- Verrucous granulomas (face), erythematous plaques and nodules.
- Biopsy of the lesions demonstrating spherules
- Musculoskeletal (bones, joints)
- One third of patients with dissemination
- Unifocal bone lesions (lytic or sclerotic, 60% of cases) and unifocal joint lesions (90% of cases, monoarticular arthritis)
- Pain and tenderness with vertebral osteomyelitis or paraspinous abscesses
- Rarely, infected tendon sheaths demonstrating a villonodular synovitis
- Hepatomegaly
- Splenomegaly
- Central nervous system
- Headache, in acute or chronic meningitis
- Acute hydrocephalus – May be the first sign of disseminated coccidioidomycosis
- Hyperreflexia (possibly)
- Cranial nerve abnormalities
Laboratory Studies
General laboratory study results are as follows:
- Normal white blood cell count or mild leukocytosis
- Peripheral eosinophilia (>5%)
- Elevation of erythrocyte sedimentation rate
Diagnosis requires isolation of the organism in culture, via histologic specimens, or with serologic testing.
- Microbiologic culture
- Isolation of C immitis from a clinical specimen establishes the diagnosis.
- Isolation can be from sputum, bronchoalveolar lavage fluid, blood, urine, bone marrow, lymph nodes, urine, skin, bone, and cerebrospinal fluid.
- The organism usually grows within 3-5 days on most routine microbiologic media.
- Laboratory personnel should handle cultures in sealed containers and with caution because the mycelial form isolated from cultures is very infectious.
- Histologic specimens
- Spherules can be seen in tissue specimens using standard stains such as hematoxylin and eosin stain or Papanicolaou stain.
- The identification of spherules on direct examination of sputum also is diagnostic but is less sensitive than cultures (sputum potassium hydroxide [KOH] smear or silver stain [Gomori methenamine silver stain]).
- Coccidioidal antibodies
- Immunoglobulin M (IgM) or precipitin antibody is detected in approximately half of all coccidioidal infections within the first week and in approximately 90% by 3 weeks. The IgM antibody fades over several weeks but may reappear under certain circumstances (eg, chronic cavitary coccidiomycosis or systemic reinfection associated with ventriculoperitoneal shunt placement. Methods of IgM detection are as follows:
- Tube precipitin – Older test and not currently in use
- Immunodiffusion tube precipitin – Better specificity; requires more time to perform than latex agglutination or enzyme immunoassay
- Latex agglutination – Rapid and highly sensitive but lacks specificity; higher false-positive rate and positive results require confirmation another test (ie, immunodiffusion tube precipitin)
- Enzyme immunoassay – Highly sensitive but lacks specificity; positive result requires confirmation immunodiffusion
- Immunoglobulin G (IgG) or complement fixation (CF) antibody appears months later and can persist for months or years. CF titers provide a quantitative measure of the immune response to infection and prognostic information with respect to dissemination. CF titers may be not be representative of the severity of infection, with lower titers occurring in patients who are immunosuppressed and unable to mount a response or in patients with overwhelming infection: Methods of IgG detection are as follows:
- Laboratory Branch complement fixation – Older test, supplanted by immunodiffusion complement fixation in most laboratories; some cross-reactivity with other dimorphic fungi
- Immunodiffusion complement fixation – Can be used to test any body fluid, including cerebrospinal fluid; increased titers indicate worsening disease; 4-fold decline in titer associated with therapeutic improvement; disseminated coccidioidomycosis associated with CF titers greater than or equal to 1:16
- Enzyme immunoassay – False positive rates limit use
- Immunoglobulin M (IgM) or precipitin antibody is detected in approximately half of all coccidioidal infections within the first week and in approximately 90% by 3 weeks. The IgM antibody fades over several weeks but may reappear under certain circumstances (eg, chronic cavitary coccidiomycosis or systemic reinfection associated with ventriculoperitoneal shunt placement. Methods of IgM detection are as follows:
- Additional assays to detection of C immitis infection are as follows:
- The urine coccidioidal antigen enzyme immunoassay was developed after cross-reactivity with the histoplasmosis urinary antigen was observed. It is useful in detecting urinary coccidioidal antigen in immunocompromised patients, but its utility in immunocompetent patients is unknown.3
- Polymerase chain reaction (PCR) assay is used to detect a target gene after DNA extraction from biopsy specimens. The utility of PCR in clinical situations is under investigation.4
- Coccidioidin and Spherulin skin tests are no longer available.
Imaging Studies
Chest radiography
The main findings on imaging can be seen on a plain chest radiograph. Typical findings found in previously described clinical syndromes are presented.
- Primary pulmonary coccidioidomycosis
- Asymptomatic patients may have a normal chest radiograph or may have residual abnormalities of a previous infection. Findings include parenchymal scarring, pleural thickening, calcified and uncalcified nodules, and lymph nodes. Calcifications occur in the minority (<15%) of lesions.
- Findings in asymptomatic patients include infiltrates (lobar, segmental, or subsegmental) indistinguishable from those seen with acute pneumonia.
- Hilar adenopathy is uncommon in bacterial pneumonia but is seen in approximately 20-25% of patients. The constellation of an infiltrate and adenopathy in a patient from an endemic area should raise suspicion for coccidioidal pneumonia. Paratracheal or mediastinal adenopathy can also be seen, and its appearance is often a precursor to disseminated disease.
- Pleural effusions can be seen in 5-15% of patients, more often left sided, transudative, and eosinophilic on analysis.
- Empyema can also occur, with diagnosis confirmed with thoracentesis.
- Bronchopleural fistulas and secondary spontaneous pneumothoraces have also been reported.
- Diffuse pneumonia is unusual and may represent a large inhalation of arthrospore or severe underlying immunodeficiency. Findings may suggest acute respiratory distress syndrome or a miliary pattern with multiple, small, bilateral nodular densities. This pattern is also seen in disseminated disease.
- Chronic pulmonary coccidioidomycosis
- Most primary coccidioidal infection resolves spontaneously, but approximately 5% of patients may develop pulmonary disease that persists beyond 3 months.
- Dense segmental and lobar consolidation, unifocal or multifocal, sometimes bilateral with cavitary regions, are the most common findings on imaging.
- Findings may resemble those seen in pulmonary tuberculosis, with associated infiltrates and fibrosis.
- Bronchiectasis may be seen in 1-2% of patients.
- Pulmonary nodules
- This is one of the most common findings on imaging and usually represents the evolution of the infiltrate to a nodule.
- Nodules can be solitary or multiple, more often in the upper lobes and usually 1-2 cm. Rarely, nodules can be as large as 6 cm.
- Calcification is uncommon, occurring in less than 15% of cases.
- Nodules may have the typical appearance of a granuloma, with smooth, well-circumscribed edges, but they can be indistinguishable from a malignant lesion.
- CT imaging may provide better definition of the nodule.
- Fluorodeoxyglucose positron-emission tomography (FDG-PET) scans may demonstrate intense uptake in nodules, similar to malignancy, but uptake may also be mild
Cavitary pulmonary coccidioidomycosis
- Cavities develop as a result of central necrosis in the granulomas or areas of consolidation.
- Cavities may be thin walled or thick walled and are seen more often in the lung apices.
- A solitary, thin-walled cavity is a common residual finding of coccidioidal infection.
- Many thin-walled cavities on plain chest radiographs are actually thick-walled cavities when visualized on CT scans.
- Cavities smaller than 2.5 cm often spontaneously resolve. Large cavities (>5 cm) may persist and be subject to hemorrhage (hemoptysis), colonization with Aspergillus (mycetoma), and pneumothorax
Disseminated pulmonary coccidioidomycosis
- Diffuse, bilateral, small nodular densities reminiscent of miliary tuberculosis can be seen in patients with overwhelming disease, either as a result of hematogenous or endobronchial spread.
- Mediastinal adenopathy is often seen as bulky paratracheal adenopathy. This is often seen in patients who are eventually diagnosed with disseminated coccidioidomycosis.
- Other manifestations seen in thoracic imaging include an enlarged cardiac silhouette representing pericardial involvement and a pericardial effusion.
Medical Care
Most patients infected with Coccidioides are asymptomatic or have self-limited symptoms that do not require more than supportive care. Symptomatic patients usually come to medical attention because of respiratory tract or systemic symptoms. Management is outlined based on previously described clinical syndromes. Most treatment recommendations represent consensus guidelines because prospective, randomized trials are lacking.
Also see the clinical guideline summary from the Infectious Diseases Society of America, Coccidioidomycosis.6
Primary pulmonary coccidioidomycosis/acute pneumonia
- No consensus has been reached on antifungal treatment for symptomatic patients.
- In endemic areas, patients with symptoms consistent with community-acquired pneumonia were found to have diagnostic coccidioidal serologies in approximately 30% of patients.7
- Patients with a higher clinical severity score and symptom score are more likely to be treated, but outcomes are not significantly different, although more complications have been seen in those with cessation of treatment.8,9
- No consensus has been reached on the duration of therapy, but 6 months of treatment is most common, and CF titers are used to monitor response to therapy.
- Risk factors for dissemination may sway the decision to treat patients, as may findings of elevated CF titers and ethnicity.
- Diffuse pneumonia warrants antifungal therapy.
Chronic progressive coccidioidal pneumonia
- Treatment is recommended with an oral azole for at least a year.
- Fluconazole at 400 mg/d and itraconazole at 200 mg twice daily appear to be equivalent in efficacy, but more patients demonstrate a response with itraconazole, which becomes evident at 12 months of therapy.
- Amphotericin B can be used for refractory infections unresponsive to oral therapy.
- Surgical resection is an option reserved for patients with refractory disease, usually those with persistent hemoptysis.
Pulmonary nodules
- Antifungal therapy is not typically recommended.
- Most lesions do not require any further investigation, especially if they are unchanged on serial imaging for 2 or more years.
- However, lesions may undergo resection if no diagnosis is established and malignancy is a concern.
Pulmonary cavities
- Asymptomatic patients often are noted incidentally. No evidence supports instituting antifungal therapy. Many resolve without specific therapy. Serial imaging can be performed to confirm stability.
- Symptomatic patients are defined by local discomfort, hemoptysis, the presence of mycetoma, or local infection. Consider treatment with oral azoles as outlined previously. Large (>5 cm) or enlarging cavities were previously treated with surgical resection after amphotericin treatment, but in current practice a trial of oral azole therapy is warranted. Surgical resection is reserved for cavities refractory to therapy or for patients with persistent complications such as hemoptysis.
- Ruptured cavities are often present as a hydropneumothorax or empyema. Chest tube drainage (if indicated) and antifungal therapy (azoles or amphotericin) are recommended in anticipation of eventual surgical resection.
Disseminated coccidioidomycosis
- Nonmeningeal coccidioidomycosis is treated with oral azoles as outlined previously. Some authors use higher doses of fluconazole (800 mg/d). Amphotericin B is recommended for rapidly progressive lesions or disease with vertebral body involvement. Vertebral involvement may also require surgical debridement and stabilization. The duration of therapy is at least a year and often longer. Changes in CF titers can help with decisions on the duration of therapy.
- Meningeal coccidioidomycosis is treated with oral fluconazole as the preferred agent. Although 400 mg/d has been reported, many treat with 800-1000 mg/d. The range for itraconazole doses is 400-600 mg. Treatment with azoles is usually life long. Hydrocephalus requires a shunt for decompression. Intrathecal amphotericin was previously used in refractory cases and initial therapy by some. The optimal dose and duration of intrathecal amphotericin unknown.
Surgical Care
Surgical resection is reserved for chronic pulmonary coccidioidal infection with severe, refractory complications including hemoptysis, bronchopleural fistula, or a failure of antifungal therapy to control symptoms.
Surgery in patients with chronic pulmonary coccidioidal infection is not uniformly curative and may result in serious complications. The potential complications of surgery include the development of postoperative bronchopleural fistula and postoperative cavity formation.
Surgical indications
- Persistent or massive hemoptysis
- Enlarging cavities (>5 cm) close to visceral pleural with high risk of rupture
- Spontaneous pneumothorax with persistent lung collapse
- Empyema drainage not amenable to chest tube drainage
- Bronchopleural fistula closure
- Expansion of lungs restricted by residual pleural disease
- Symptomatic fungus ball
Limitations to surgical treatment
- High complication rate with closure of bronchopleural fistula (30%)
- Recurrent disease (cavitation) in 18%
- Reduced postoperative risk seen with preoperative amphotericin B therapy, but experience with azole therapy unknown
Consultations
- Pulmonary and infectious disease specialists
- Surgeon in select cases
Diet
No specific diet is necessary for patients with coccidioidal infection.
Activity
No specific limitations in activity are necessary for patients with coccidioidal infection. Any limitations would be as a result of the adverse effects of the infection as it relates to hemodynamics, respiratory status, stamina, and ambulation.
Medication
Amphotericin B, fluconazole, and itraconazole are the antifungal agents currently recommended as first-line agents for the treatment of coccidioidal infection. Ketoconazole is efficacious, but has been largely replaced by fluconazole. Relapses have been reported in 7-39% of patients. Initial oral therapy should be with either fluconazole (400 mg/d) or itraconazole (200 mg bid), with higher doses in patients with disseminated disease or meningitis.
The duration of therapy is dictated by the clinical course of the illness, but it should be at least 6 months in all patients and often a year or longer in others. Therapy is tailored based on a combination of resolution of symptoms, regression of radiographic abnormalities, and changes in CF titers. Patients with a history of meningeal involvement require lifelong treatment.
No studies have directly compared amphotericin B with azole therapy. Amphotericin B should be considered as initial therapy in patients with rapidly progressive or life-threatening disease and in pregnant patients. Posaconazole, voriconazole, and caspofungin are under investigation as alternative agents and as possible alternatives for refractory coccidioidal infection.
- Ketoconazole
- First oral broad-spectrum antifungal medication
- Moderate activity for coccidioidomycosis
- Treatment response rate of 12-32%
- High rate of recurrence with medication discontinuation
- Higher dose with significant adverse effects
- Risk for reduced testosterone synthesis
- Itraconazole
- Variable absorption levels depending on acidic gastric pH
- Absorption impaired by agents that alter gastric pH such as proton pump inhibitors
- Itraconazole study group with skeletal infections responded twice as fast as fluconazole group; difference between groups not statistically significant[19]
- Fluconazole
- Standard treatment used in coccidioidal infection
- Efficacy in life-long treatment of coccidioidal meningitis
- Sometimes used in combination with intrathecal amphotericin B for treatment of coccidioidal meningitis
- Amphotericin B
- Lipid-based formulation preferred because of reduced renal toxicity
- Indicated in rapidly progressive disease
- Indicated in pregnancy because of the presumed teratogenicity of azoles
- Posaconazole
- Structurally similar to itraconazole
- Highly active in vitro against C immitis
- Trial information: In an open-label, multicenter, international study, patients with invasive coccidioidal disease refractory to standard therapy (amphotericin with or without azoles) were treated with posaconazole; 11 of 15 patients had treatment success.10 The study was limited by a small sample size, poor patient compliance, significant baseline treatment differences, and nonrandomized study design.
- Trial information: A small study in an open-label trial showed 5 of 6 successful treatment outcomes in patients with disseminated coccidioidomycosis in whom conventional antifungal treatment failed.11
- Other cases of treatment success reported12
- More study needed prior to consideration for treatment of refractory coccidioidal infection
- Voriconazole
- Few reported cases of use in salvage therapy13
- More study needed prior to consideration
- Caspofungin
- Echinocandin
- Few reported cases of success14
- More study needed prior to consideration
Antifungals
Their mechanism of action may involve increasing the permeability of the cell membrane, which in turn causes intracellular components to leak.
Posaconazole (Noxafil)
Triazole antifungal agent. Blocks ergosterol synthesis by inhibiting the enzyme lanosterol 14-alpha-demethylase and sterol precursor accumulation. This action results in cell membrane disruption. Available as oral susp (200 mg/5 mL). Indicated for prophylaxis of invasive Aspergillus and Candida infections in patients at high risk because of severe immunosuppression.
- Dosing
- Interactions
- Contraindications
- Precautions
Adult
400 mg PO qd with food or liquid nutritional supplement to enhance absorption
Pediatric
<12 years: Not established
>12 years: Administer as in adults
- Dosing
- Interactions
- Contraindications
- Precautions
Metabolized via UDP glucuronidation; P-gp efflux substrate; CYP3A4 inhibitor
UDP-G inducers (eg, rifabutin, phenytoin) and drugs that increase gastric pH (eg, cimetidine) decrease serum levels (avoid concomitant use unless benefit outweighs risk)
Inhibits CYP3A4 and may elevate serum levels of cyclosporine, tacrolimus, sirolimus, rifabutin, midazolam, phenytoin, calcium channel blockers (eg, nifedipine, bepridil), HMG-CoA reductase inhibitors (eg, lovastatin, pravastatin), ergot alkaloids, terfenadine, astemizole, cisapride, pimozide, halofantrine, quinidine, or vinca alkaloids (eg, vincristine, vinblastine)
- Dosing
- Interactions
- Contraindications
- Precautions
Documented hypersensitivity; coadministration with ergot alkaloids; coadministration with CYP3A4 substrates (eg, terfenadine, astemizole, cisapride, pimozide, halofantrine, quinidine) likely to result in serious toxicities
- Dosing
- Interactions
- Contraindications
- Precautions
Pregnancy
C – Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Common adverse effects include nausea, vomiting, diarrhea, rash, hypokalemia, thrombocytopenia, and elevated liver enzyme levels; closely monitor patients with severe diarrhea or vomiting for breakthrough fungal infections; rare adverse events include arrhythmias caused by QTc prolongation, bilirubinemia, or liver function impairment; caution with preexisting cardiac risk factors (eg, history of arrhythmia, hypokalemia, hypomagnesemia); food improves absorption and provides optimal serum concentration; shake well before use; administer with measuring spoon provided in package; avoid if breastfeeding
Voriconazole (VFEND)
Used for primary treatment of invasive aspergillosis and salvage treatment of Fusarium species or Scedosporium apiospermum infections. A triazole antifungal agent that inhibits fungal CYP450-mediated 14 alpha-lanosterol demethylation, which is essential in fungal ergosterol biosynthesis.
- Dosing
- Interactions
- Contraindications
- Precautions
Adult
Loading dose: 6 mg/kg IV q12h infused over 2 h for 2 doses
Maintenance: 4 mg/kg IV q12h infused over 2 h, when able to tolerate PO may switch to 200 mg PO q12h
Note: For inadequate response, may increase to 300 mg PO q12h; <40 kg administer oral maintenance dose of 100 mg PO q12h (may increase to 150 mg PO q12h)
Pediatric
Not established
- Dosing
- Interactions
- Contraindications
- Precautions
CYP450 2C19 (highest affinity), 2C9, and 3A4 (minor) substrate and inhibitor; CYP450 inducers (eg, rifampin) have shown to decrease steady state peak plasma levels by up to 93%; may increase serum levels of drugs metabolized by CYP450 2C19 or 2C9, of which some are contraindicated (eg, sirolimus, pimozide, quinidine, cisapride, ergot alkaloids), other may need more frequent monitoring (eg, cyclosporine, tacrolimus, warfarin, HMG CoA inhibitors, benzodiazepines, calcium channel blockers)
- Dosing
- Interactions
- Contraindications
- Precautions
Documented hypersensitivity; do not administer IV form with CrCl <50 mL/min (decreased excretion of IV vehicle); coadministration with rifampin, rifabutin, carbamazepine, barbiturates, sirolimus, pimozide, quinidine, cisapride, ergot alkaloids
- Dosing
- Interactions
- Contraindications
- Precautions
Pregnancy
D – Fetal risk shown in humans; use only if benefits outweigh risk to fetus
Precautions
Decrease maintenance dose with hepatic dysfunction; common adverse effects include visual disturbances, fever, rash, vomiting, nausea, diarrhea, headache, sepsis, peripheral edema, abdominal pain, rash (including Stevens-Johnson Syndrome and phototoxicity), and respiratory disorder; rare cases of severe hepatotoxicity have been reported; administer PO 1 h ac or pc
Caspofungin (Cancidas)
Used to treat refractory invasive aspergillosis. First of a new class of antifungal drugs (glucan synthesis inhibitors). Inhibits synthesis of beta-(1,3)-D-glucan, an essential component of fungal cell wall.
- Dosing
- Interactions
- Contraindications
- Precautions
Adult
70 mg IV infused over 1 h on day 1; 50 mg IV qd thereafter
Pediatric
<3 months: Not established
3 months to 18 years: 70 mg/m2 IV infused over 1 h on day 1; 50 mg/m2/d IV thereafter; not to exceed 70 mg/d for either loading dose or maintenance dose
>18 years: Administer as in adults
- Dosing
- Interactions
- Contraindications
- Precautions
Coadministration with cyclosporine may increase risk of hepatotoxicity; carbamazepine, nelfinavir, efavirenz, or dexamethasone may decrease levels of caspofungin; caspofungin may decrease levels of tacrolimus; rifampin decreases caspofungin levels by 30% (ie, adjust dose to 70 mg/d)
- Dosing
- Interactions
- Contraindications
- Precautions
Documented hypersensitivity
- Dosing
- Interactions
- Contraindications
- Precautions
Pregnancy
C – Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Caution in moderate hepatic dysfunction (ie, decrease dose to 35 mg/d); may exacerbate preexisting renal dysfunction or myelosuppression
Ketoconazole (Nizoral)
Imidazole broad-spectrum antifungal agent. Inhibits synthesis of ergosterol, causing cellular components to leak, resulting in fungal cell death.
- Dosing
- Interactions
- Contraindications
- Precautions
Adult
200-400 mg PO qd
Pediatric
Not established
- Dosing
- Interactions
- Contraindications
- Precautions
Isoniazid may decrease bioavailability; coadministration decreases effects of either rifampin or ketoconazole; may increase effect of anticoagulants; may increase toxicity of corticosteroids and cyclosporine (cyclosporine dosage can be adjusted); may decrease theophylline levels
- Dosing
- Interactions
- Contraindications
- Precautions
Documented hypersensitivity; fungal meningitis
- Dosing
- Interactions
- Contraindications
- Precautions
Pregnancy
C – Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Hepatotoxicity may occur; may reversibly decrease corticosteroid serum levels (adverse effects avoided with dose of 200-400 mg/d); administer antacids, anticholinergics, or H2 blockers at least 2 h after taking ketoconazole
Itraconazole (Sporanox)
Oral antifungal agent with broad-spectrum antifungal activity. Decreases ergosterol synthesis and inhibits cell membrane formation.
- Dosing
- Interactions
- Contraindications
- Precautions
Adult
200 mg PO bid
Pediatric
Not established
- Dosing
- Interactions
- Contraindications
- Precautions
Antacids may reduce absorption; edema may occur with coadministration of calcium channel blockers (eg, amlodipine, nifedipine); hypoglycemia may occur with sulfonylureas; may increase tacrolimus and cyclosporine plasma concentrations when high doses are used; rhabdomyolysis may occur with coadministration of HMG-CoA reductase inhibitors (lovastatin, simvastatin); coadministration with cisapride can cause cardiac rhythm abnormalities and death; may increase digoxin levels; coadministration may increase plasma levels of midazolam or triazolam; phenytoin and rifampin may reduce itraconazole levels (phenytoin metabolism may be altered)
- Dosing
- Interactions
- Contraindications
- Precautions
Documented hypersensitivity; coadministration with cisapride may cause adverse cardiovascular effects (possibly death)
- Dosing
- Interactions
- Contraindications
- Precautions
Pregnancy
C – Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Caution in hepatic insufficiencies; adverse effects include nausea (common), fatigue, malaise, rash, abdominal pain, and hepatitis
Fluconazole (Diflucan)
Synthetic oral antifungal (broad-spectrum bistriazole) that selectively inhibits fungal cytochrome P-450 and sterol C-14 alpha demethylation.
- Dosing
- Interactions
- Contraindications
- Precautions
Adult
200-400 mg PO qd
Pediatric
3-6 mg/kg PO qd for 14-28 d depending on severity of infection
- Dosing
- Interactions
- Contraindications
- Precautions
Levels may increase with hydrochlorothiazides; fluconazole levels may decrease with long-term coadministration of rifampin; may increase concentrations of theophylline, phenytoin, tolbutamide, cyclosporine, glyburide, and glipizide; effects of anticoagulants may increase with fluconazole coadministration
- Dosing
- Interactions
- Contraindications
- Precautions
Documented hypersensitivity
- Dosing
- Interactions
- Contraindications
- Precautions
Pregnancy
C – Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Closely monitor patients who develop rashes during treatment and discontinue if lesions progress; may cause clinical hepatitis, cholestasis, and fulminant hepatic failure (including fatalities), especially when a serious underlying medical condition (eg, AIDS, malignancy) is present and often while taking multiple concomitant medications
Amphotericin B (AmBisome)
Depending on the concentration attained in body fluids and on fungal susceptibility, can be fungistatic or fungicidal. Polyene antibiotic produced by a strain of Streptomyces nodosus that changes membrane permeability by binding to sterols in the fungal cell membrane. Fungal cell death results.
- Dosing
- Interactions
- Contraindications
- Precautions
Adult
0.5-1 mg/kg/d IV; not to exceed 2-4 g/dose
Pediatric
2.5 mg/kg/d IV