paronychia
Paronychia is a soft tissue infection around a fingernail. Paronychia occurs in 2 forms: acute and chronic. The etiology, infectious agent, and treatment are usually different for each form, and the 2 forms are often considered separate entities.
Pathophysiology
Mechanism
Paronychia, whether acute or chronic, results from a breakdown of the protective barrier between the nail and the nail fold. The entry of organisms into the moist nail crevice results in the bacterial or fungal (yeast or mold) colonization of the area.
The anatomy of the nail complex is shown in the image below. The nail is longitudinally flanked by 2 lateral folds or perionychium. Proximally, it is covered by the eponychium. Distal to the perionychium, the region immediately beneath the free edge of the nail is the hyponychium. The hyponychium serves as a tough physical barrier that resists bacterial infection.
The nail or nail plate lies immediately on top of the nail bed, which consists of 2 portions involved in the production, migration, and maintenance of the nail. The proximal portion, called the germinal matrix, contains active cells that are responsible for generating new nail. Damage to the germinal matrix results in malformed nails. The distal portion, the sterile matrix, adds thickness, bulk, and strength to the nail. The white crescent-shaped opacity at the proximal end of the nail is the lunula, which is the visible portion of the germinal matrix. The whiteness of the lunula is due to the poor vascularity of the germinal matrix. The nail arises from a mild proximal depression called the nail fold. The nail divides the nail fold into 2 components: the dorsal roof and the ventral floor, both of which contain germinal matrices. The skin overlying the nail fold is called the nail wall.
The nail bed receives its blood supply from the 2 terminal branches of the volar digital artery. A fine network in the proximal nail bed and in the skin proximal to the nail fold of the finger provides venous drainage. Lymphatic drainage follows a course similar to that of the venous network. The lymphatic network is dense in the nail bed, especially in the hyponychium. Innervation is derived from the trifurcation of the dorsal branch of the volar digital nerve. One branch goes to the nail fold, one to the pulp, and one to the distal tip of the finger.
The patient’s history is crucial in determining the possibility of more serious underlying systemic conditions that may predispose the patient to paronychia. These underlying conditions may include diabetes, obesity, hyperhidrosis, immunologic defects, polyendocrinopathy, and drug-induced immunosuppression. Note the following:
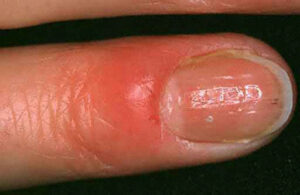
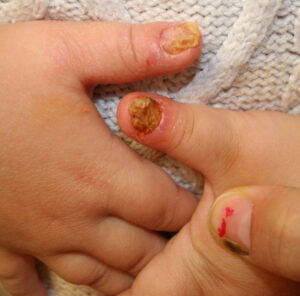
- Acute paronychia: Patients with acute paronychia often present with a history of minor trauma to the fingertip or nail manipulation, intentional or not. The presenting complaints are pain, tenderness, and swelling in one of the lateral folds of the nail.
- Chronic paronychia: Generally, patients report symptoms lasting 6 weeks or longer. Inflammation, pain, and swelling may occur episodically, often after an exposure to water or a moist environment.
Physical
Acute paronychia physical findings are as follows:
- The affected area often appears erythematous and swollen.
- In more advanced cases, pus may collect under the skin of the lateral fold.
- If untreated, the infection can extend into the eponychium, in which case, it is called eponychia.
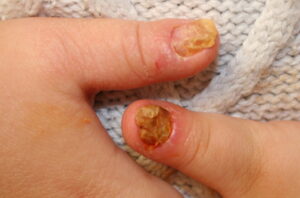
- Further extension of the infection can lead to the involvement of both lateral folds as it tracks under the nail sulcus; this progression is called a runaround infection.
- In severe cases, the infection may track proximally under the skin of the finger and volarly to produce a concomitant felon. The fulminant purulence of the nail bed may generate enough pressure to lift the nail off the nail bed.
Chronic paronychia physical findings are as follows:
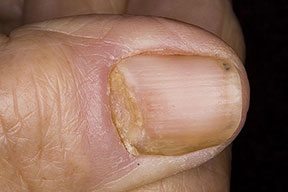
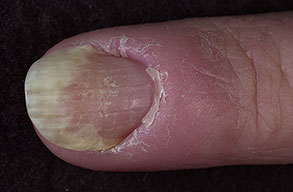
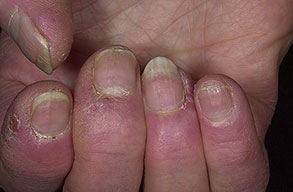
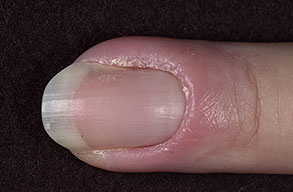
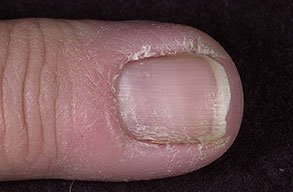
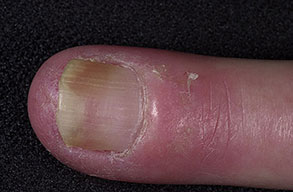
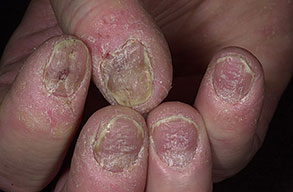
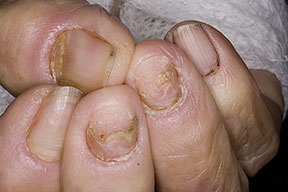
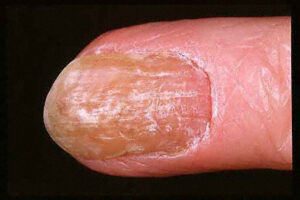
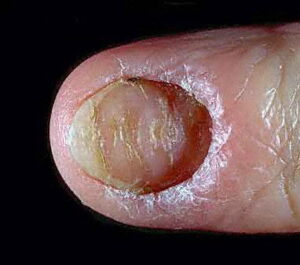
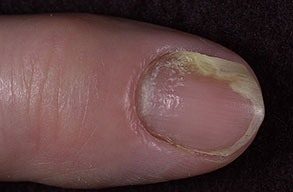
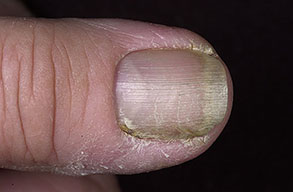
- Swollen, erythematous, and tender nail folds without fluctuance are characteristic of chronic paronychia.
- Eventually, the nail plates become thickened and discolored, with pronounced transverse ridges.
- The cuticles and nail folds may separate from the nail plate, forming a space for the invasion of various microorganisms.
Causes
Acute paronychia causes are as follows:
- Acute paronychia usually results from a traumatic event, however minor, that breaks down the physical barrier between the nail bed and the nail; this disruption allows the infiltration of infectious organisms.
- Acute paronychia can result from seemingly innocuous conditions, such as hangnails, or from activities, such as nail biting, finger sucking, manicuring, or artificial nail placement.
- Staphylococcus aureus is the most common infecting organism. Organisms, such as Streptococcus and Pseudomonas species, gram-negative bacteria, and anaerobic bacteria are other causative organisms.
- Acute (and chronic) paronychia may also occur as a manifestation of other diseases, such as pemphigus vulgaris. Although instances of nail involvement in pemphigus vulgaris are rare, they can be severe, involving multiple digits and hemorrhage.
Chronic paronychia causes are as follows:
- Chronic paronychia is primarily caused by the yeast fungus Candida albicans.
- Other rare causes of chronic paronychia include bacterial, mycobacterial, or viral infection; metastatic cancer; subungual melanoma; squamous cell carcinoma; and Raynaud disease. Therefore, benign and malignant neoplasms should always be excluded when chronic paronychia does not respond to conventional treatment.
- Chronic paronychia most often occurs in persons whose hands are repeatedly exposed to moist environments or in those who have prolonged and repeated contact with irritants such as mild acids, mild alkalis, or other chemicals. People who are most susceptible include housekeepers, dishwashers, bartenders, and swimmers.
Other conditions associated with abnormalities of the nail fold that predispose individuals to chronic paronychia include psoriasis, mucocutaneous candidiasis, and drug toxicity from medications such as retinoids, epidermal growth factor receptor inhibitors (cetuximab), and protease inhibitors.1,2 Of particular interest is the antiretroviral drug indinavir, which induces retinoidlike effects and remains the most frequent cause of chronic paronychia in patients with HIV disease.
Laboratory Studies
Fluctuant paronychia is usually caused by bacteria; therefore, routine Gram staining helps in identifying the organism.
Potassium hydroxide 5% smears may be helpful in diagnosing fluctuant paronychia if Gram staining results are negative or if candidal infection is suspected, as in chronic paronychia. If Gram staining results are positive, the KOH preparation may demonstrate pseudomycelia and clusters of grapelike yeast cells. KOH wet mounts from scrapings or discharge may show hyphae.
Tzanck smears may be performed if herpetic whitlow is suspected. Smears should be performed by using base scrapings of an unroofed vesicle. The presence of multinucleated giant cells, often with visible viral inclusions, indicates a positive result.
Imaging Studies
No radiologic studies are required. The diagnosis is primarily based on the features of the history and on the physical examination findings.
Medical Care
The treatment of choice depends on the extent of the infection. If diagnosed early, acute paronychia without obvious abscess can be treated nonsurgically. If an abscess has developed, incision and drainage must be performed. Surgical debridement may be required if fulminant infection is present.
Herpetic whitlow and paronychia must be distinguished because the treatments are drastically different. Misdiagnosis and mistreatment may do more harm than good. Once herpetic whitlow is ruled out, one must determine whether the paronychia is acute or chronic and then treat it accordingly.5
Acute paronychia
Warm water soaks of the affected finger 3-4 times per day until symptoms resolve are helpful.
Oral antibiotics with gram-positive coverage against S aureus, such as amoxicillin and clavulanic acid (Augmentin) or clindamycin (Cleocin), are usually administered concomitantly with warm water soaks. Cleocin and Augmentin also have anaerobic activity; therefore, they are useful in treating patients with paronychia due to oral anaerobes contracted through nail biting or finger sucking. Cleocin should be used instead of Augmentin in patients who are allergic to penicillin.
If the paronychia does not resolve or if it progresses to an abscess, it should be drained promptly.
Chronic paronychia
The initial treatment of chronic paronychia consists of the avoidance of inciting factors such as exposure to moist environments or skin irritants. Keeping the affected lesion dry is essential for proper recovery. Choice of footgear may also be considered.
Any manipulation of the nail, such as manicuring, finger sucking, or attempting to incise and drain the lesion, should be avoided; these manipulations may lead to secondary bacterial infections.
Mild cases of chronic paronychia may be treated with warm soaks.
The initial medical treatment consists of the application of topical antifungal agents. Topical miconazole may be used as the initial agent. Oral ketoconazole or fluconazole may be added in more severe cases.
Patients with diabetes and those who are immunocompromised need more aggressive treatment because the response to therapy is slower in these patients than in others.
In cases induced by retinoids or protease inhibitors, the paronychia usually resolves if the medication is discontinued.
Surgical Care
If paronychia does not resolve despite best medical efforts, surgical intervention may be indicated. Also, if an abscess has developed, incision and drainage must be performed. Surgical debridement may be required if fulminant infection is present.
Acute paronychia
The no-incision technique is as follows:
- Less advanced paronychial abscesses can be drained simply by gently elevating the eponychial fold from the nail by using a small blunt instrument such as a metal probe or an elevator (see the images below). This separation is performed at the junction of the perionychium and the eponychium and extends proximally enough to permit visualization of the proximal nail edge. Then, the proximal third of the nail can be excised with scissors and the pus evacuated.
- This technique does not require an incision into the matrix. Often, no excision of any tissues is made because only blunt dissection and separation are needed to evacuate the pus from the paronychia.
- The wound should be well irrigated with isotonic sodium chloride solution, and plain gauze packing should be inserted under the fold to keep the cavity open and allow drainage.
- The patient should receive oral antibiotics for 5-7 days.
- The packing is removed after 2 days, and warm sodium chloride solution soaks are begun
The single- and double-incision techniques are as follows:
- If the paronychia is more advanced, it may need to be incised and drained.
- A digital anesthetic block is usually necessary. If an anesthetic agent is used, it should consist of 1% lidocaine (Xylocaine) with no epinephrine for a ring block. The local injection of the anesthetic agent into the paronychia or the wound is often inadequate and more painful than the administration of drugs of a digital ring block.
- If the paronychia involves only 1 lateral fold of the finger, a single longitudinal incision should be placed with either a number-11 or a number-15 blade directed away from the nail fold to prevent proximal injury with a subsequent nail growth abnormality. If both lateral folds of the finger are involved, incisions may be made on both sides of the nail, extending proximally to the base of the nail.
- After the single or double incision is made, the entire eponychial fold is elevated to expose the base of the nail and drain the pus.
- The proximal third of the nail is removed by using the technique described for the no-incision technique.
- After the abscess is drained, the pocket should be well irrigated with isotonic sodium chloride solution, packed with plain packing, and dressed.
- The patient should receive oral antibiotics for 5-7 days.
- The dressing and packing are removed in approximately 2 days, and the affected finger is treated with warm soaks for 10-15 minutes 3-4 times per day.
Chronic paronychia
Treatment is as follows:
- The most common surgical technique used to treat chronic paronychia is called eponychial marsupialization.
- In this technique, the affected digit is first anesthetized with 1% lidocaine (Xylocaine) with no epinephrine by using the digital ring block method.
- Tourniquet control of the proximal digit is accomplished by using a finger of a latex glove with the distal end cut off.
- With a No. 15 blade, a crescent-shaped incision is made proximal to the distal edge of the eponychial fold.
- The distal incision is made approximately 1 mm proximal to the distal edge of the eponychium and along its curve.
- At its widest end, the proximal incision is approximately 5 mm from the distal incision.
- The incision should appear symmetric and extend to the edge of the nail fold on each side.
- All affected tissue within the boundaries of the crescent and extending down to, but not including, the germinal matrix is excised. In effect, this procedure exteriorizes the infected and obstructed nail matrix and allows its drainage.
- If the nail plate is grossly deformed at the time of surgery, it may be removed.
- The excised region is packed with plain gauze wick, which is changed every 2-3 days.
- Epithelialization of the excised defect occurs over the next 2-3 weeks.
- Nail improvement occurs over the next 6-9 months but may require as long as 12 months to become apparent