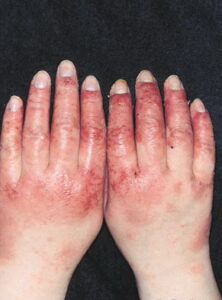
Acute contact dermatitis= التهاب الجلدالحاد بالتماس
Acute contact dermatitis
Contact dermatitis is any inflammatory reaction of the skin that results from direct contact with an offending agent. Most cases of contact dermatitis evaluated in the ED can be classified as allergic contact dermatitis (ACD) (see the image below) or irritant contact dermatitis (ICD). Additional types of contact dermatitis seen in the ED include photodermatitis and contact urticaria
Pathophysiology
The main pathologic feature of contact dermatitis is intercellular edema of the epidermis. This initial reaction may result in intraepidermal vesicle and bullae formation in acute cases and papules, scaling, and lichenification in chronic cases. Within the dermal layer, various cells congregate around the dilated capillaries to aid in inflammatory response.
Irritant contact dermatitis (ICD) results from direct injury to the skin. It affects individuals exposed to specific irritants and generally produces a stinging or burning sensation within seconds of exposure. Alternatively, extended exposure to a mild irritant can cause a chronic form of ICD. In this case, dryness precipitates an erythematous state, which ultimately leads to cracking and the formation of painful fissures.
Allergic contact dermatitis affects only individuals previously sensitized to the contactant. It represents a delayed (cell-mediated, type IV) hypersensitivity reaction and classically requires several hours to complete the cascade of cellular immunity before symptoms manifest
History
- In acute allergic contact dermatitis (ACD), lesions appear within 24-96 hours of exposure to the allergen.
- The main symptom, in addition to the lesion, is pruritus.
- Location of the dermatitis is helpful in identifying the cause.
- Most heavily contaminated areas break out first, followed by areas of lesser exposure.
- In more severe ACD reactions, lesions can form in adjacent areas of the skin that never had direct contact with the offending agent.
- Irritant contact dermatitis (ICD) is divided into 2 types.
- Mild irritants require prolonged or repeated exposure before inflammation is noted.
- Strong irritants (eg, strong acids, alkalis) can produce immediate reactions similar to thermal burns.
- Unlike ACD, ICD will only erupt in areas of the skin that have had direct contact with the irritant.
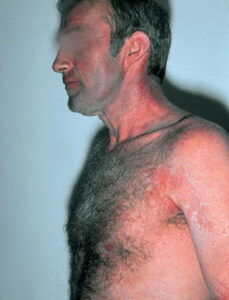
- Photodermatitis is diagnosed by the presence of lesions limited to sun-exposed body areas.
- Burning is the primary complaint in phototoxic reactions.
- Pruritus is the main complaint in photoallergic reactions.
- Skin contact with photosensitizing agents found in some plants (notably limes) followed by ultraviolet (UV) irradiation can precipitate a type of photodermatitis called phytophotodermatitis.
- Contact urticaria reactions occur within 1 hour of exposure to the inciting agent.
Physical
- Most cases of contact dermatitis have a similar appearance regardless of the mechanism or cause of inflammation. Inflammatory responses can be categorized into acute, subacute, and chronic phases. In all phases, a key feature is localization to the area of contact.
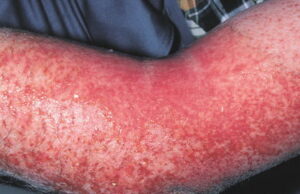
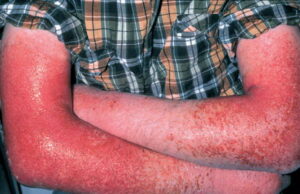
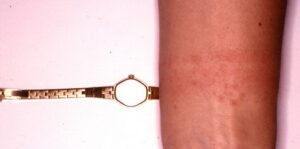
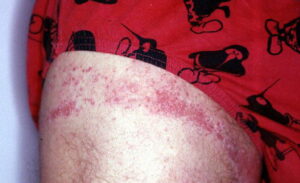
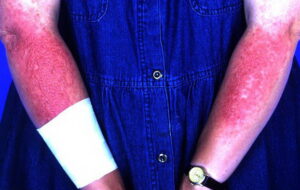
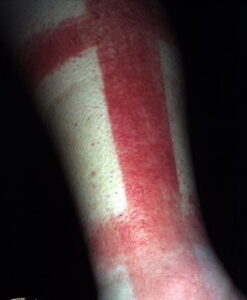
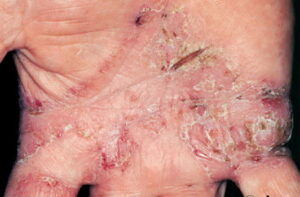
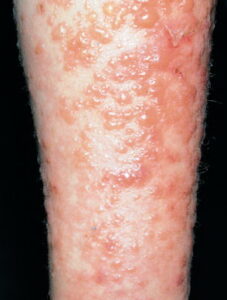
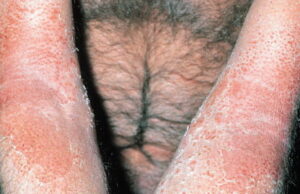
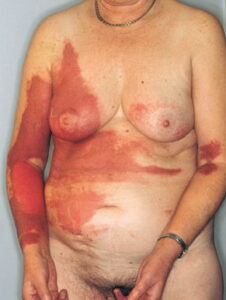
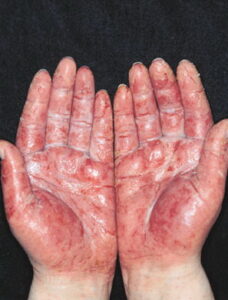
- Acute contact dermatitis presents with bright red edematous skin (see the first image below). In moderate-to-severe cases, clear fluid-filled vesicles or bullae appear (see the second image below). As the lesions break, skin becomes exudative and weeps clear fluid. In acute ICD, these lesions and surrounding erythema are sharply demarcated and located in the distribution of the area of contact
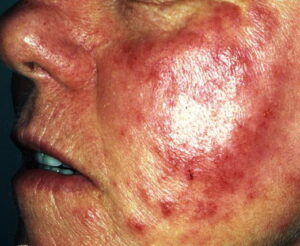
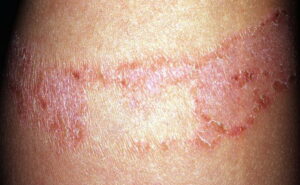
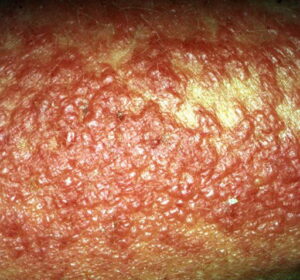
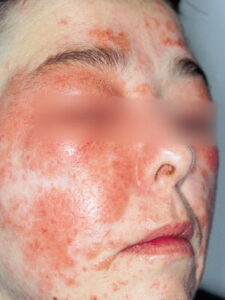
- Subacute contact dermatitis is characterized by the formation of papules instead of the vesicles more typical of the acute phase (see the image below). Additionally, less edema is seen in the subacute phase. Dry scales are sometimes seen in subacute contact dermatitis.
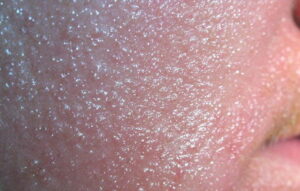
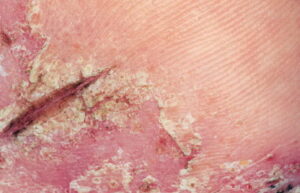
- Chronic contact dermatitis presents with scaling, skin fissuring, and lichenification but only minimal edema. Excoriations can also be observed in chronic contact dermatitis.
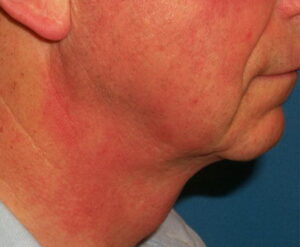
- Contact urticaria has a wheal-and-flare response at the site of exposure.
Causes
Causes of contact dermatitis are classified into 4 groups according to mechanism of response: allergic contact dermatitis, irritant contact dermatitis, photodermatitis, and contact urticaria.
- Allergic contact dermatitis
- A cell-mediated type IV delayed hypersensitivity reaction results from specific antigens penetrating the epidermal skin layer. The antigen combines with a protein mediator and travels to the dermis, where T lymphocytes become sensitized. On the subsequent exposure to the antigen, the allergic reaction takes place.
- Contributing factors include allergen concentration, duration of exposure, and presence of other skin diseases.
- The most common agents are plants of the Toxicodendron genus (eg, poison ivy, poison oak, poison sumac).
- Other substances include nickel sulfate (various metal alloys), sunscreens, potassium dichromate (cements, household cleaners), formaldehyde, ethylenediamine (dyes, medications), mercaptobenzothiazole (rubbers), thiram (fungicides), and paraphenylenediamine (dyes, photographic chemicals).4
- Repeated exposures to an ACD-inducing allergen tend to cause incrementally more severe reactions.
- Irritant contact dermatitis
- An irritant produces direct local cytotoxic effect on the cells of the epidermis, with a subsequent inflammatory response in the dermis.
- The most common site is the hand.
- Individuals with atopic dermatitis have an inborn constitutional skin weakness. The risk of developing irritant contact dermatitis is particularly high in individuals with eczema affecting the hands.
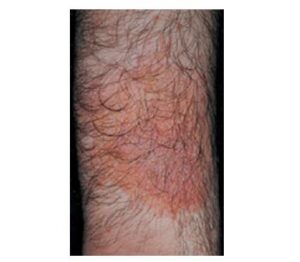
- Although irritant contact dermatitis is caused mostly by chemicals (eg, acids, alkalis, solvents, oxidants, rubber, latex), plants (eg, hot peppers, garlic, tobacco) have also been implicated.5,6 See the image below
- Severity of the reaction is related to the amount and duration of exposure to the irritant.
- Most cases of ICD are acute in onset, in which symptoms develop within seconds of exposure.
- Alternatively, prolonged exposure to a low-level irritant can lead to chronic ICD. Soaps and prolonged exposure to water, often due to occupational soaking of the hands, are typical causes of chronic ICD.2
- Photodermatitis
- Irradiation of certain substances by ultraviolet light results in the transformation of the substance into allergens (photoallergic) or irritants (phototoxic).
- A common example of this is phytophotodermatitis, in which a phototoxic reaction occurs after skin that has been in contact with citrus fruit (or another plant contact) is exposed to sunlight. This exposure to sun chemically alters a previously benign agent in citrus (called furocoumarin or psoralen) into a skin allergen.
- Many plant families are known to cause a phototoxic response. Besides citrus, these plant families include mulberry (figs) and Umbelliferae (parsnip, celery).
- Medications (particularly sulfa drugs, thiazides, tetracycline) have also been implicated in photodermatitis.
- Contact urticaria (immunologic, nonimmunologic)
- Immunologic reaction is a type I IgE-mediated process caused by the immediate release of inflammatory mediators, resulting in a wheal-and-flare reaction. In rare cases, anaphylactic shock can result. Foodstuffs and latex have been implicated.
- Nonimmunologic contact urticaria results in local edema and erythema. It is more common than the immunologic mechanism. Substances containing benzoic, sorbic, cinnamic, or nicotinic acids often are the cause.
- Allergic contact dermatitis
- .
Laboratory Studies
- Laboratory examination of allergic contact dermatitis (ACD) focuses on patch testing. In this examination, a dermatologist or an allergist applies multiple potential allergens into the skin of the patient. The presence of erythema, papules, or vesicles can indicate a positive test. Patch testing is most accurate several weeks after the resolution of the dermatitis, and thus has no role in the ED.
Imaging Studies
- No ED imaging studies are of value in diagnosing contact dermatitis.
Other Tests
- Patch testing may be beneficial to identify the contact allergen and is usually performed in an outpatient setting.
Procedures
- Pathologic findings obtained from biopsy specimens include intercellular edema and bullae
Treatment
Emergency Department Care
- General measures
- The definitive treatment of both irritant contact dermatitis (ICD) and allergic contact dermatitis (ACD) is the identification and removal of any potential causal agents.
- Topical soaks with cool tap water, Burow solution (1:40 dilution), saline (1 tsp/pint), or silver nitrate solution (25.5%)
- Lukewarm water baths (antipruritic)
- Aveeno (oatmeal) baths
- Emollients (eg, white petrolatum, Eucerin) may be beneficial chronic cases.
- Large vesicles may benefit from therapeutic drainage (but not removing the vesicle tops).1 These lesions should then be covered with dressing soaked in Burow solution.
- General measures
Practice guidelines are available from the American Academy of Allergy, Asthma, and Immunology, and the American College of Allergy, Asthma, and Immunology.8
Consultations
Patients with recurrent episodes of contact dermatitis or rash of unclear etiology may benefit from an outpatient dermatologic consultation.
Medication
Treatment of contact dermatitis depends on the type (irritant or allergic), extent, and area of skin lesions on initial presentation. Preventative advice is as important as the prescription of medications. Once an allergen or irritant is identified as the cause of contact dermatitis, eliminate further exposure.
Wet compresses with an astringent
These compresses are soothing, have a mild antipruritic effect, and keep affected areas clean.
Aluminum acetate (Burow solution)
Dissolve aluminum acetate tabs in water for a 1:40 solution.
- Dosing
- Interactions
- Contraindications
- Precautions
Adult
Apply as compress for 20-30 min 4-6 times/d
Pediatric
Apply as in adults
- Dosing
- Interactions
- Contraindications
- Precautions
None reported
- Dosing
- Interactions
- Contraindications
- Precautions
Documented hypersensitivity
- Dosing
- Interactions
- Contraindications
- Precautions
Pregnancy
A – Fetal risk not revealed in controlled studies in humans
Precautions
For external use only
Topical steroids
Topical steroids are the mainstay of treatment of contact dermatitis. Topical agents of medium-to-high strength (class I-IV) should be adequate to treat most cases. In general, ointments are preferred over creams.
Triamcinolone acetate (Aristocort)
Treats inflammatory dermatosis responsive to steroids. Decreases inflammation by suppressing the migration of polymorphonuclear leukocytes and reversing capillary permeability. A moderate potency is available in both ointment (0.1%) and cream (0.5%).
- Dosing
- Interactions
- Contraindications
- Precautions
Adult
Apply tid initially; reduce as lesions remit
Pediatric
Apply as in adults
- Dosing
- Interactions
- Contraindications
- Precautions
None reported
- Dosing
- Interactions
- Contraindications
- Precautions
Documented hypersensitivity; fungal, viral, and bacterial skin infections
- Dosing
- Interactions
- Contraindications
- Precautions
Pregnancy
C – Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Multiple complications (eg, severe infections, hyperglycemia, edema, osteonecrosis, myopathy, peptic ulcer disease, hypokalemia, osteoporosis, euphoria, psychosis, myasthenia gravis, growth suppression) may occur; abrupt discontinuation of glucocorticoids may cause adrenal crisis
Hydrocortisone valerate 0.2% (LactiCare HC, DermaGel, Cortaid, Dermacort)
Lower-potency cream useful on the face. An adrenocorticosteroid derivative suitable for application to skin or external mucous membranes. Has mineralocorticoid and glucocorticoid effects resulting in anti-inflammatory activity.
- Dosing
- Interactions
- Contraindications
- Precautions
Adult
Apply tid initially; reduce as lesions remit
Pediatric
Apply as in adults
- Dosing
- Interactions
- Contraindications
- Precautions
None reported
- Dosing
- Interactions
- Contraindications
- Precautions
Documented hypersensitivity; viral, fungal, and bacterial skin infections
- Dosing
- Interactions
- Contraindications
- Precautions
Pregnancy
C – Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Prolonged use, applying over large surface areas, applying potent steroids, and using occlusive dressings may increase systemic absorption of corticosteroids and may cause Cushing syndrome, reversible HPA axis suppression, hyperglycemia, and glycosuria
Systemic steroids
Use in severe cases that involve more than 10-20% of total body surface area (TBSA) or bullae. Systemic therapy may also be considered when sleep or activities of daily living are impaired.1 They have both anti-inflammatory (glucocorticoid) and salt-retaining (mineralocorticoid) properties. Glucocorticoids cause profound and varied metabolic effects. In addition, these agents modify the body’s immune response to diverse stimuli.
Prednisone (Deltasone, Orasone, Sterapred)
Used for treatment of a variety of diseases, including adrenocortical insufficiency. Prednisone is inactive and must be metabolized to the active metabolite prednisolone. Conversion may be impaired in patients with liver disease. Use for 2-3 weeks with taper. Too short a course results in recurrence of lesions.
- Dosing
- Interactions
- Contraindications
- Precautions
Adult
50 mg PO qd for 1 wk; taper by a 10-mg reduction in dose q3d
Pediatric
1 mg/kg PO for 1 wk; taper by a 20% reduction in dose q3d; available in 5 mg/5 mL elixir (prednisolone sodium phosphate); prolonged use in children can suppress growth
- Dosing
- Interactions
- Contraindications
- Precautions
Coadministration with estrogens may decrease prednisone clearance; concurrent use with digoxin may cause digitalis toxicity secondary to hypokalemia; phenobarbital, phenytoin, and rifampin may increase metabolism of glucocorticoids (consider increasing maintenance dose); monitor for hypokalemia with coadministration of diuretics
- Dosing
- Interactions
- Contraindications
- Precautions
Documented hypersensitivity; viral, fungal, tubercular skin, or connective tissue infections; peptic ulcer disease; hepatic dysfunction; GI disease
- Dosing
- Interactions
- Contraindications
- Precautions
Pregnancy
C – Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Abrupt discontinuation of glucocorticoids may cause adrenal crisis; hyperglycemia, edema, osteonecrosis, myopathy, peptic ulcer disease, hypokalemia, osteoporosis, euphoria, psychosis, myasthenia gravis, growth suppression, and infections may occur with glucocorticoid use
Antihistamines
These agents may be used as adjuncts to relieve pruritus associated with contact dermatitis.
Diphenhydramine (Benadryl)
Used for the symptomatic relief of allergic symptoms caused by histamine released in response to allergens.
- Dosing
- Interactions
- Contraindications
- Precautions
Adult
25-50 mg cap PO q6h prn
Pediatric
5 mg/kg/d (12.5 mg/5 mL elixir) PO divided qid
- Dosing
- Interactions
- Contraindications
- Precautions
Potentiates effect of CNS depressants; because of alcohol content, do not give syrup dosage form to patients taking medications that can cause disulfiramlike reactions
- Dosing
- Interactions
- Contraindications
- Precautions
Documented hypersensitivity; glaucoma; prostatic hypertrophy
- Dosing
- Interactions
- Contraindications
- Precautions
Pregnancy
C – Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
May exacerbate angle-closure glaucoma, hyperthyroidism, peptic ulcer, and urinary tract obstruction
Hydroxyzine HCl (Atarax, Vistaril)
Antagonizes H1 receptors in the periphery and may be used as alternative to diphenhydramine. May also suppress histamine activity in subcortical region of the CNS. Available in 10 mg/5 mL elixir.
- Dosing
- Interactions
- Contraindications
- Precautions
Adult
25-50 mg PO tid/qid prn
Pediatric
<6 years: 30-50 mg/d PO divided tid
>6 years: 50-100 mg/d PO divided tid- Dosing
- Interactions
- Contraindications
- Precautions
CNS depression may increase with alcohol or other CNS depressants
- Dosing
- Interactions
- Contraindications
- Precautions
Documented hypersensitivity
- Dosing
- Interactions
- Contraindications
- Precautions
Pregnancy
C – Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Associated with clinical exacerbations of porphyria (may not be safe for patients with porphyria); ECG abnormalities (alterations in T waves) may occur; may cause drowsiness
Emollients
These agents may be used as adjuncts to moisturize dry skin in subacute and chronic contact dermatitis.
Urea cream (Ureacin, Ureaphil)
Promotes hydration and removal of excess keratin in conditions of hyperkeratosis.
- Dosing
- Interactions
- Contraindications
- Precautions
Adult
Apply to affected area prn
Pediatric
Apply as in adults
- Dosing
- Interactions
- Contraindications
- Precautions
None reported
- Dosing
- Interactions
- Contraindications
- Precautions
Documented hypersensitivity; viral skin disease
- Dosing
- Interactions
- Contraindications
- Precautions
Pregnancy
C – Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Do not use near eyes; caution if applied to broken or swollen skin
Mineral oil (Fleet, Zymenol)
Promotes removal of excess keratin in conditions of hyperkeratosis.
- Dosing
- Interactions
- Contraindications
- Precautions
Adult
Apply to affected area prn
Pediatric
Administer as in adults
- Dosing
- Interactions
- Contraindications
- Precautions
None reported
- Dosing
- Interactions
- Contraindications
- Precautions
Documented hypersensitivity
- Dosing
- Interactions
- Contraindications
- Precautions
Pregnancy
C – Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Observe for hypersensitivity reactions
Barrier creams
These are the primary agents for diaper dermatitis.
Zinc oxide paste (Desitin)
Provides relief of minor skin irritations.
- Dosing
- Interactions
- Contraindications
- Precautions
Adult
Not established
Pediatric
Apply to affected area after gentle cleansing and drying, between each diaper change
- Dosing
- Interactions
- Contraindications
- Precautions
None reported
- Dosing
- Interactions
- Contraindications
- Precautions
Documented hypersensitivity
- Dosing
- Interactions
- Contraindications
- Precautions
Pregnancy
C – Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Observe for hypersensitivity reactions
Dry skin agents
Moisturize dry skin in subacute and chronic contact dermatitis.
Camphor and menthol (0.5% each) in emollient base (Sarna Anti-Itch)
Topical drug combination that consists of mild local anesthetics, counterirritants, and antipruritic formulations. Generally safe and effective for symptomatic relief.
- Dosing
- Interactions
- Contraindications
- Precautions
Adult
Apply to affected area prn
Pediatric
<12 years: Not established
>12 years: Apply as in adults