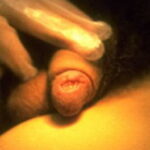
Syphilis
Treponema pallidum is the microaerophilic spirochete that causes syphilis, a chronic systemic venereal disease with multiple clinical presentations (often referred to as “the great imitator”). Syphilis is characterized by episodes of active disease (primary, secondary, tertiary stages) interrupted by periods of latency. Since the diagnosis frequently is suspected after examination of skin lesions, dermatologists are recognized as experts in the diagnosis and treatment of syphilis. Syphilis can be transmitted either by intimate contact with infectious lesions (most common) or via blood transfusion (if blood has been collected during early syphilis). The disease can also be transmitted transplacentally from an infected mother to her fetus.
Pathophysiology
In acquired syphilis, the organism rapidly penetrates intact mucous membranes or microscopic dermal abrasions and, within a few hours, enters the lymphatics and blood to produce systemic infection. The CNS is invaded early in the infection; during the secondary stage, examinations demonstrate that more than 30% of patients have abnormal findings in the cerebrospinal fluid (CSF). During the first 5-10 years after the onset of untreated primary infection, the disease principally involves the meninges and blood vessels, resulting in meningovascular neurosyphilis. Later, the parenchyma of the brain and spinal cord are damaged, resulting in parenchymatous neurosyphilis.
Regardless of the stage of disease and location of lesions, histopathologic hallmarks of syphilis include endarteritis (which in some instances may be obliterative in nature) and a plasma cell–rich infiltrate. Endarteritis is caused by the binding of spirochetes to endothelial cells, mediated by host fibronectin molecules bound to the surface of the spirochetes. The resultant endarteritis can heal with scarring in some instances.
The syphilitic infiltrate reflects a delayed-type hypersensitivity response to T. pallidum, and in certain individuals with tertiary syphilis, this response by sensitized T lymphocytes and macrophages results in gummatous ulcerations and necrosis. Antigens of T. pallidum induce host production of treponemal antibodies and nonspecific reagin antibodies. Immunity to syphilis is incomplete. For example, host humoral and cellular immune responses may prevent the formation of a primary lesion (chancre) on subsequent infections with T pallidum, but they are insufficient to clear the organism. This may be because the outer sheath of the spirochete is lacking immunogenic molecules, or it may be because of down-regulation of helper T cells of the TH1 class.1
- Although rarely seen by clinicians since the use of penicillin became widespread in the 1950s, the primary complications of syphilis in adults include neurosyphilis, cardiovascular syphilis, and gumma. Death resulting from syphilis continues to occur. One study found that of 113 recorded deaths resulting from sexually transmitted diseases, 105 were caused by syphilis, with cardiovascular and neurosyphilis accounting for the majority of these deaths.
- These figures have continued to increase since the emergence of the AIDS epidemic, since genital ulcer diseases (including syphilis) are cofactors for the sexual transmission of HIV. Additionally, untreated patients who are HIV seropositive have an increased risk for rapid progression to neurosyphilis and for its complications. In addition, patients with HIV are at greater risk for development or relapse of early symptomatic neurosyphilis for up to 2 years after treatment with intramuscular or intravenous penicillin.
- Congenital syphilis is the most serious outcome of syphilis in women. It has been shown that a higher proportion of infants are affected if the mother has untreated secondary syphilis, compared to untreated early latent syphilis. Since T pallidum does not invade the placental tissue or the fetus until the fifth month of gestation, syphilis causes late abortion, stillbirth, or death soon after delivery in more than 40% of untreated maternal infections.5,6 Neonatal mortality usually results from pulmonary hemorrhage, bacterial superinfection, or fulminant hepatitis.
,2
History
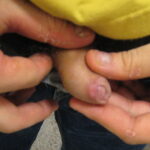
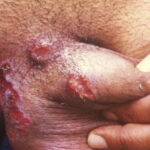
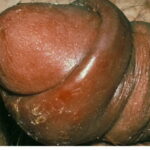
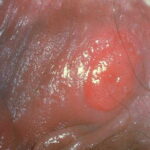
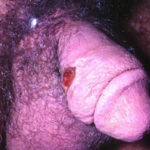
- Primary syphilis occurs within 3 weeks of contact with an infected individual. Patients usually present with a solitary red papule that rapidly forms a painless nonbleeding ulcer or chancre (see Media File 1). The chancre usually heals within 4-8 weeks, with or without therapy.
- Secondary syphilis usually presents with a cutaneous eruption within 2-10 weeks after the primary chancre and is most florid 3-4 months after infection. The eruption may be subtle; 25% of patients may be unaware of skin changes.
- Mild constitutional symptoms of malaise, headache, anorexia, nausea, aching pains in the bones, and fatigue often are present, as well as fever and neck stiffness.
- A small number of patients develop acute syphilitic meningitis and present with headache, neck stiffness, facial numbness or weakness, and deafness.
- The lesions of benign tertiary syphilis usually develop within 3-10 years of infection. The typical lesion is a gumma, and patient complaints usually are secondary to bone pain, which is described as a deep boring pain characteristically worse at night. Trauma may predispose a specific site to gumma involvement.
- CNS involvement may occur, with presenting symptoms representative of the area affected, ie, brain involvement (headache, dizziness, mood disturbance, neck stiffness, blurred vision) and spinal cord involvement (bulbar symptoms, weakness and wasting of shoulder girdle and arm muscles, incontinence, impotence).
- Some patients may present up to 20 years after infection with behavioral changes and other signs of dementia, which is indicative of neurosyphilis.
- A small percentage of infants infected in utero may have a latent form of infection that becomes apparent during childhood and, in some cases, during adult life. The earliest symptom that occurs prior to age 2 years is rhinitis (snuffles), soon followed by cutaneous lesions. After age 2 years, parents may note problems with the child’s hearing and language development and with vision. Facial and dental abnormalities may be noted.
Physical
- Primary syphilis
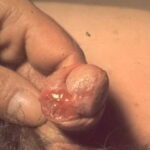
- The primary lesion (chancre) occurs on the penis or scrotum of 70% of men with syphilis and on the vulva, cervix, or perineum of more than 50% of women with syphilis.
- The primary lesion usually is a single ulcerated lesion with a surrounding red areola. The edge and base of the ulcer have a cartilaginous (buttonlike) consistency on palpation.
- The lesion is highly infectious; when abraded, it exudes a clear serum containing numerous T pallidum organisms.
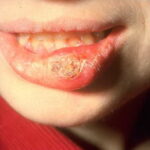
- Extragenital chancres occur most commonly above the neck, typically affecting the lips or oral cavity.
- The regional lymph nodes usually enlarge painlessly and are firm, discrete, and nontender.
- Secondary syphilis
- The protean manifestations of the secondary stage usually include localized or diffuse symmetric mucocutaneous lesions and generalized nontender lymphadenopathy
- The healing primary chancre may remain present in 15-25% of patients.
- Initial lesions are bilaterally symmetric, pale red to pink (in light-skinned persons) or pigmented (in dark-skinned persons), discrete, round macules that measure 5-10 mm in diameter and are distributed on the trunk and proximal extremities.
- After several days or weeks, red papular lesions 3-10 mm in diameter appear. These lesions often become necrotic and are distributed widely with frequent involvement of the palms and soles.
- Tiny papular follicular syphilids involving hair follicles may result in patchy alopecia. In addition to the classic moth-eaten alopecia, a diffuse alopecia also has been reported.
- Primary syphilis
- In 10% of patients, highly infectious papules develop at the mucocutaneous junctions and, in moist intertriginous skin, become hypertrophic and dull pink or gray
- From 10-15% of patients with secondary syphilis develop superficial mucosal erosions on the palate, pharynx, larynx, glans penis, vulva, or in the anal canal and rectum. These mucous patches are circular silver-gray erosions with a red areola.
- Ocular abnormalities, such as iritis, are a rare clinical finding, although anterior uveitis has been reported in 5-10% of patients with secondary syphilis.
- Less common findings include periostitis, arthralgias, meningitis, nephritis, hepatitis, and ulcerative colitis.
- Tertiary syphilis
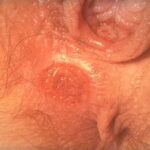
- Gummas may be identified on the skin, in the mouth, and in the upper respiratory tract. They appear most commonly on the leg just below the knee.
- Gummas may be multiple or diffuse but usually are solitary lesions that range from less than 1 cm to several centimeters in diameter.
- Cutaneous gummas are indurated, nodular, papulosquamous or ulcerative lesions that form characteristic circles or arcs with peripheral hyperpigmentation.
- The most common clinical finding on cardiovascular examination is a diastolic murmur with a tambour quality, secondary to aortic dilation with valvular insufficiency.
- Symptomatic neurosyphilis produces various clinical syndromes that develop in approximately 5% of patients with syphilis who remain untreated. The most common presentation of meningovascular syphilis (diffuse inflammation of the pia and arachnoid along with widespread arterial involvement) is an indolent stroke syndrome involving the middle cerebral artery.
- Cranial nerve palsies and pupillary abnormalities occur with basilar meningitis.
- Argyll Robertson pupil, which occurs almost exclusively in neurosyphilis, is a small irregular pupil that reacts normally to accommodation but not to light.
- Tabes dorsalis presents with signs of demyelination of the posterior columns, dorsal roots, and dorsal root ganglia (eg, ataxic wide-based gait and foot slap, areflexia and loss of position, deep pain and temperature sensations). Deep ulcers of the feet can result from loss of pain sensation.
- Rare findings include iritis, with possible adhesion of the iris to the anterior lens, producing a fixed pupil (not to be confused with Argyll Robertson pupil).
- Congenital syphilis: The manifestations of untreated congenital syphilis can be divided into those that are expressed prior to age 2 years (early) or after age 2 years (late).
- Early manifestations9
- Early signs and symptoms include development of a diffuse rash, characterized by extensive sloughing of the epithelium, particularly on the palms, soles, and skin around the mouth and anus.
- A compilation of early clinical presentations of congenital syphilis in 9 studies involving a total of 212 infants included abnormal bone radiographs (61%), hepatomegaly (51%), splenomegaly (49%), petechiae (41%), other skin rashes (35%), anemia (34%), lymphadenopathy (32%), jaundice (30%), pseudoparalysis (28%), and snuffles (23%).
- A classic mucocutaneous sign is depressed linear scars radiating from the orifice of the mouth and termed rhagades (Parrot lines).
- Late manifestations10
- Late signs and symptoms are rare and, if encountered, usually involve complications including interstitial keratitis, cranial nerve VIII deafness, corneal opacities, and/or recurrent arthropathy.
- The clinical manifestations of untreated congenital neurosyphilis present in 25% of patients older than age 6 years and correspond to those of adult neurosyphilis.
- Gummatous periostitis occurs in patients aged 5-20 years and tends to cause destructive lesions of the palate and nasal septum (saddle nose).
- Dental abnormalities may be evident, such as centrally notched and widely spaced, peg-shaped, upper central incisors (Hutchinson teeth) and sixth-year molars with multiple poorly developed cusps (mulberry molars).
- Peculiar bone findings include frontal bossing of Parrot and Higoumenakia sign, which is unilateral irregular enlargement of the sternoclavicular portion of the clavicle secondary to periostitis.
Laboratory Studies
- In suspected acquired syphilis, perform nontreponemal serology screening using Venereal Disease Research Laboratory (VDRL), rapid plasma reagin (RPR), or the recently developed ICE Syphilis recombinant antigen test. Then, test sera yielding a positive or equivocal reaction by the fluorescent treponemal antibody-absorption (FTA-ABS), quantitative VDRL/RPR, and microhemagglutination assay Treponema pallidum (MHA-TP) tests.11,12
- Dark-field microscopy is essential in evaluating moist cutaneous lesions, such as the chancre of primary syphilis or the condyloma lata of secondary syphilis. When dark-field microscopy is not available, direct immunofluorescence staining of fixed smears (direct fluorescent antibody Treponema pallidum [DFA-TP]) is an option. Both procedures detect the causative organism at a rate of approximately 85-92%.
- For evaluation of infants with suspected congenital syphilis, the 19S immunoglobulin M FTA-ABS serology test or the Captia Syphilis-M test currently is recommended. Every pregnant woman should undergo a nontreponemal test at her first prenatal visit, and women at high risk of exposure should have a repeat test in the third trimester and again at delivery.
- The US Preventive Services Task Force has reaffirmed its recommendation for screening all pregnant women for syphilis infection at the first prenatal visit. High-risk women (eg, uninsured women, women living in poverty, sex workers, illicit drug users, those with other sexually transmitted diseases, those living in communities with high syphilis morbidity) should also be tested in the third trimester and at delivery. If test results are positive for syphilis, the treatment of choice is parenteral benzathine penicillin G. Dosage and the length of treatment depend on the stage and clinical manifestations of the disease.13
Imaging Studies
- Radiologic abnormal findings commonly seen with advanced gummas of bone include periostitis, destructive osteitis, or sclerosing osteitis.
- For cardiovascular complications of tertiary syphilis, linear calcification of the ascending aorta on chest films suggests asymptomatic syphilitic aortitis.
- Angiography may be useful to distinguish between abdominal aneurysms of syphilitic versus arteriosclerotic origin since 10% of syphilitic aneurysms occur superior to the renal arteries, while arteriosclerotic abdominal aneurysms usually are found inferior to the renal arteries.
Other Tests
- Echocardiogram and ECG may help confirm cardiovascular syphilis.
Procedures
- Biopsy may be necessary to differentiate gummas from coincidental granulomatous conditions.
- Lumbar puncture for CSF examination is indicated in the following situations: neurologic signs or symptoms, treatment failure or plans to administer treatment other than penicillin, a serum reagin titer of greater than or equal to 1:32, seropositive HIV, and other changes indicative of active syphilis (eg, gumma, aortitis). Additionally, the only means by which the occurrence of asymptomatic neurosyphilis in latent syphilis can be excluded is via CSF examination.
Histologic Findings
- Primary syphilis: Skin and mucosal lesions show a perivascular and perijunctional infiltrate of lymphocytes, plasma cells, and macrophages. At times, capillary endothelial proliferation and subsequent obliteration of small blood vessels may be appreciable. Focal erosion or ulceration is common.
- Secondary syphilis: Skin lesions are typified by a “lichenoid-psoriasiform” configuration with a perijunctional infiltrate of lymphocytes, histiocytes, and plasmacytes. Often the histiocytic component of the infiltrate is prominent and thus the biopsy may assume a “lichenoid-granulomatous” configuration. Small numbers of neutrophils may be included in the perijunctional infiltrate, and neutrophils may also be present in an expanded overlying stratum corneum. Organisms are readily demonstrable using T pallidum immunoperoxidase staining during the secondary stage.
- Tertiary lesions: Gummas consist of granulomatous inflammation with central necrosis flanked by plump or palisaded macrophages and fibrocytes surrounded by large numbers of mononuclear leukocytes, including many plasma cells. Treponemes may be scant in gummas and are sometimes difficult to demonstrate. Aortitis reveals inflammatory scarring of the tunica media, secondary to obliterative endarteritis of the vasa vasorum. Uneven loss of the medial elastic fibers and muscle cells may be evident
Medical Care
Penicillin remains the mainstay of treatment and the standard by which other modes of therapy are judged.14
- Penicillin use is the only therapy used widely for neurosyphilis, congenital syphilis, or syphilis during pregnancy. Rarely, T pallidum has been found to persist following adequate penicillin therapy; however, there is no indication that the organism has acquired resistance to penicillin.
- In patients with allergy to penicillin, skin testing and desensitization are recommended. Make every effort to document penicillin allergy before choosing an alternative treatment because the efficacy of alternative regimens is questionable in all stages of syphilis. Many treatment failures have been reported.
- Tetracycline, erythromycin, and ceftriaxone have shown antitreponemal activity in clinical trials; however, they currently are recommended only as alternative treatment regimens in patients allergic to penicillin.
Consultations
Consultations are necessary depending on the specific complications and organ systems affected.
Medication
Penicillin is the mainstay of treatment, the standard by which other modes of therapy are judged, and the only therapy that has been used widely for neurosyphilis, congenital syphilis, or syphilis during pregnancy. On rare occasions, T pallidum has been found to persist after adequate penicillin therapy; however, no indication exists that T pallidum has acquired resistance to the drug.
Tetracycline, erythromycin, and ceftriaxone have shown antitreponemal activity in clinical trials but currently are recommended only as alternative treatment regimens in patients allergic to penicillin.
Antibiotics
Empiric antimicrobial therapy must be comprehensive and should cover all likely pathogens in the context of the clinical setting.
Penicillin G benzathine (Bicillin LA)
Interferes with synthesis of cell wall mucopeptides during active multiplication, which results in bactericidal activity.
Adult
Disease for <1 year: 2.4 million U IM once in 2 injection sites
Disease for >1 year: 2.4 million U in 2 injection sites qwk for 3 doses
Neurosyphilis: Aqueous crystalline penicillin G at 18-24 million U/d, administered as 3-4 million U IV q4h or continuous infusion, for 10-14 dPediatric
Disease for <1 year: 50,000 U/kg IM once; not to exceed 2.4 million U
Disease for >1 year: 50,000 U/kg IM qwk for 3 doses; not to exceed 2.4 million UProbenecid can increase penicillin effectiveness by decreasing clearance; coadministration with tetracyclines can decrease effectiveness of penicillin
Documented hypersensitivity
Pregnancy
B – Fetal risk not confirmed in studies in humans but has been shown in some studies in animals
Precautions
Jarisch-Herxheimer reaction (syndrome of influenzalike symptoms) may follow initiation of penicillin treatment, usually subsiding within 24 h; however, patients with syphilitic general paresis or high CSF cell count may experience serious complications, including seizures, hemiplegia, or monoplegia
Tetracycline (Sumycin)
Alternative agent for penicillin-allergic patients. Treats gram-positive and gram-negative organisms as well as mycoplasmal, chlamydial, and rickettsial infections. Inhibits bacterial protein synthesis by binding with 30S and possibly 50S ribosomal subunit(s).
Adult
Primary, secondary, and early latent disease: 500 mg PO qid for 14 d
Late latent syphilis with normal CSF, cardiovascular syphilis, and late benign (gumma) disease: 500 mg PO qid for 28 dPediatric
<8 years: Not recommended
>8 years: 25-50 mg/kg/d (10-20 mg/lb) PO qidBioavailability decreases with antacids containing aluminum, calcium, magnesium, iron, or bismuth subsalicylate; can decrease effects of oral contraceptives, causing breakthrough bleeding and increased risk of pregnancy; tetracyclines can increase hypoprothrombinemic effects of anticoagulants
Documented hypersensitivity; severe hepatic dysfunction; pregnancy (hepatotoxicity to mother, transplacental to fetus); breastfeeding
Pregnancy
D – Fetal risk shown in humans; use only if benefits outweigh risk to fetus
Precautions
Photosensitivity may occur with prolonged exposure to sunlight or tanning equipment; reduce dose in renal impairment; consider drug serum level determinations in prolonged therapy; tetracycline use during tooth development (last one-half of pregnancy through age 8 y) can cause permanent discoloration of teeth; Fanconilike syndrome may occur with outdated tetracyclines
Erythromycin (E.E.S., E-Mycin, Eryc)
Alternative agent for penicillin-allergic patients. Inhibits bacterial growth, possibly by blocking dissociation of peptidyl t-RNA from ribosomes causing RNA-dependent protein synthesis to arrest. For treatment of staphylococcal and streptococcal infections.
In children, age, weight, and severity of infection determine proper dosage. When bid dosing is desired, half-total daily dose may be taken q12h. For more severe infections, double the dose.Adult
250 mg stearate/base (or 400 mg ethylsuccinate) PO q6h or 500 mg q12h
Pediatric
Not recommended
30-50 mg/kg/d PO in divided doses; consider double dosing for neurologic involvementCoadministration may increase toxicity of theophylline, digoxin, carbamazepine, and cyclosporine; may potentiate anticoagulant effects of warfarin; coadministration with lovastatin and simvastatin increases risk of rhabdomyolysis
Documented hypersensitivity; hepatic impairmen
Pregnancy
B – Fetal risk not confirmed in studies in humans but has been shown in some studies in animals
Precautions
Caution in liver disease; estolate formulation may cause cholestatic jaundice; adverse GI effects are common (give doses pc); discontinue use if nausea, vomiting, malaise, abdominal colic, or fever occur
Ceftriaxone (Rocephin)
Alternative agent for penicillin-allergic patients. Third-generation cephalosporin with broad-spectrum, gram-negative activity; lower efficacy against gram-positive organisms; higher efficacy against resistant organisms. Arrests bacterial growth by binding to one or more penicillin binding proteins.
Adult
2 gm qd IM/IV for 10-14 d
Pediatric
Not recommended
75-100 mg/kg IV/IM qd for 10-14 d
- Early manifestations9