Erythema toxicum neonatorum
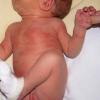
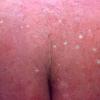
Erythema toxicum neonatorum (ETN) is a benign self-limited eruption occurring primarily in healthy newborns in the early neonatal period. Erythema toxicum neonatorum is characterized by macular erythema, papules, vesicles, and pustules, and it resolves without permanent sequelae.1 Also see the eMedicine Pediatrics article, Erythema Toxicum.
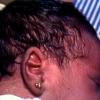
Increased levels of immunological and inflammatory mediators (eg, interleukins 1 and 8, eotaxin, the adhesion molecule E-selectin, the water-channel proteins aquaphorin 1 and aquaphorin 3, the chemotactic factor psoriasin, high-mobility group box chromosomal protein 1, nitric oxide and its isoforms, the antimicrobial peptide LL-37) suggest that erythema toxicum neonatorum may be an immune system reaction.2,3,4 The location of erythema toxicum neonatorum to primarily hair-bearing areas suggests that the hair follicle may be involved. Additionally, the number of mast cells is increased around hair follicles in involved skin.5
The eosinophilic infiltrate of erythema toxicum neonatorum suggests an allergic- or hypersensitivity-related etiology, but no allergens have been identified. Newborn skin appears to respond to any injury with an eosinophilic infiltrate. Because erythema toxicum neonatorum is rarely seen in premature infants, it is believed that mature newborn skin is required to produce this reaction pattern.6
Contactants and mechanical irritation have been considered and rejected as etiologies
History
When evaluating for erythema toxicum neonatorum (ETN), focus the history on age at onset of the eruption, absence of systemic signs (eg, fever, irritability, lethargy, mucocutaneous involvement), or maternal history of herpes simplex/varicella viral infection, bacterial pyoderma, or candidiasis.
- Infants with erythema toxicum neonatorum otherwise are healthy and lack systemic symptoms.
- The eruption is self-limited with most cases resolving within 5-14 days without residual sequelae.
- Recurrences are uncommon but have been reported up to the sixth week of life. They tend to be mild in severity.
Physical
Focus the physical examination on location, size, and distribution of macules, wheals, papules, and pustules on the skin. Note the absence of mucosal, palmar, or plantar involvement. Signs of systemic toxicity, including hypothermia or hyperthermia, lethargy, and irritability, are not associated with erythema toxicum neonatorum.
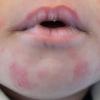
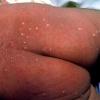
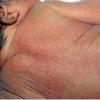
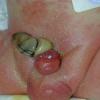
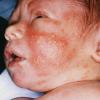
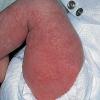
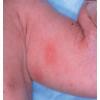
- Erythema toxicum neonatorum most commonly presents with a blotchy, evanescent, macular erythema, often on the face or trunk.
- The macules are irregular, blanchable, and vary in size.
- In more severe cases, pale yellow or white wheals or papules on an erythematous base may follow. In approximately 10% of patients, 2-4 mm pustules develop.
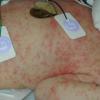
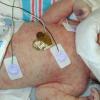
- Numbers and distribution of lesions vary from a few and widely scattered to numerous and extensive.
- Sites of predilection include the forehead, face, trunk, and proximal extremities, but lesions may occur anywhere, including the genitalia.13 Involvement of the mucous membranes and palms and soles rarely occurs.
Causes
The cause of erythema toxicum neonatorum is unknown. Multiple theories have been proposed to explain this common disorder.
- Neonates have an increased number of hair follicles compared with adults, and the occurrence of erythema toxicum neonatorum in non–hair-bearing areas such as palms and soles is rare. Inflammatory cells tend to concentrate around hair follicles, and coccilike microbes have been demonstrated in the follicular epithelium and inside the inflammatory cells. This suggests that erythema toxicum neonatorum may be a response to microbes that have penetrated the hair follicle. This process may possibly be integral in developing the new immune system.14
- The high frequency of eosinophilia suggests an allergic basis, leading some authors to suggest that erythema toxicum neonatorum may be an immediate hypersensitivity reaction to a substance passed from the mother transplacentally; however, convincing support is lacking for this theory.15
- No responsible exotoxin, allergen, component of sebum, or infectious agent has been linked credibly to erythema toxicum neonatorum.
- Medications administered to newborns and the mode of feeding have no effect on incidence.
- Other proposed theories include a transient adjustment reaction of the skin to mechanical or thermal stimulation or an acute graft-versus-host reaction induced by the maternal-fetal transfer of lymphocytes before or during delivery.16 Analysis of skin samples of 2 male patients with erythema toxicum neonatorum did not support a graft-versus-host reaction because no maternal cells were found in the samples using fluorescence in situ hybridization identification of cells with 2 XX chromosomes.17
- Risk factors include birth in hot wet climates, being fed on a mixed diet or milk-powder substitute, and being born via vaginal delivery. A positive correlation has been recognized between the length of labor and both the incidence of erythema toxicum neonatorum and the duration of the cutaneous manifestations
Laboratory Studies
- Erythema toxicum neonatorum (ETN) is diagnosed clinically based on history, physical examination, and peripheral smear of intralesional contents.
- On a CBC count, eosinophilia are noted in approximately 15% of patients as up to 18% of the total WBC count. Eosinophilia may be more pronounced when the eruption shows a marked pustular component.
- A Tzanck smear or Gram stain performed on intralesional contents is essential for diagnosis. Inflammatory cells are present, with greater than 90% eosinophils and variable numbers of neutrophils.19
Other Tests
- Perform viral, bacterial, and fungal cultures to exclude herpes simplex virus, varicella, pathogenic bacterial, and yeast infections.
- Perform potassium hydroxide preparation to exclude candidiasis.
Procedures
- A skin biopsy is diagnostic but rarely is required for diagnosis.
Histologic Findings
Histologic examination of macules reveals mild dermal edema with a sparse predominantly perivascular inflammatory infiltrate composed primarily of eosinophils, with small numbers of neutrophils and monocytes. Papules have increased edema and inflammatory infiltrate with involvement of the superficial portion of the pilosebaceous unit. Eosinophilic invasion of the outer root sheath of the hair follicle is noted. Pustules are subcorneal or intraepidermal and are found associated with the pilosebaceous orifice. A variable infiltrate of eosinophils and monocytes may be seen with or without neutrophils in the surrounding dermis.
Medical Care
Erythema toxicum neonatorum (ETN) diagnosis rests on recognizing the characteristic history and physical findings in an otherwise healthy newborn.
- A complete history, physical examination, and Tzanck smear are required to differentiate between benign transient pustular eruptions of the newborn and life-threatening disease.
- Erythema toxicum neonatorum is a benign self-limited disorder requiring no treatment. Reassure parents regarding the benign transitory nature of the condition.
Most erythema toxicum neonatorum (ETN) cases resolve within 3-4 days after onset without residua.
Rare recurrences are seen in a small number of patients up to age 6 weeks. In these instances, follow-up examination may be needed

