Eosinophilic cellulitis (Wells syndrome)
In 1971, George Wells first described this syndrome as a recurrent granulomatous dermatitis with eosinophilia.1 Wells and Smith renamed it eosinophilic cellulitis in 1979.2
Eosinophilic cellulitis (Wells syndrome) is an uncommon condition of unknown etiology. The presentation usually involves a mildly pruritic or tender cellulitislike eruption with typical histologic features characterized by edema, flame figures, and a marked infiltrate of eosinophils in the dermis.3 Papular and nodular eruptions at the clinical presentation have also been reported.4,5 The condition can recur and may be preceded by a pruritic papular eruption. Although Wells syndrome is usually sporadic, some familial cases have been reported.
One study showed the successive occurrence of vasculitis, Wells syndrome, and Sweet syndrome in a patient. This finding suggests that an overlap between these diseases exists.6 Another report describes a dominant syndrome consisting of eosinophilic cellulitis, mental retardation, and abnormal body habitus in one family.7
Pathophysiology
The etiology is unknown. At least some cases may represent hypersensitivity to an arthropod bite or sting. A dermal infiltrate of histiocytes, eosinophils, and eosinophilic granules occurs between collagen bundles, which forms the classic flame figures. The eosinophilic infiltrate is almost always restricted to the epidermis and the dermis, but it has also been found in the subcutaneous tissue and the underlying muscle. The location of the infiltrate is correlated with the different clinical features.
In one study, immunophenotyping of peripheral T cells revealed an increased proportion of CD3+ and CD4+ T cells.8 These lymphocytes spontaneously release significant amounts of interleukin 5 (IL-5); this finding suggests that activated T cells may be involved in the pathogenesis of blood and tissue eosinophilia. The eosinophils then degranulate in the dermis, causing edema and inflammation.9
With immunofluorescent stains, eosinophil major basic protein is identified in the granules of the flame figures. On electron microscopy, the collagen fibers are intact; this finding suggests that an initial degeneration of collagen is not a factor in initiating the formation of flame figures.
Eosinophilic cellulitis may be due to drugs, various infections, and, possibly, nonhematological malignancies as trigger events.10,11 Wells syndrome has also been reported to occur in patients with hypereosinophilic syndrome and Churg-Strauss syndrome.
History
Usually, the patient reports pruritus or a burning sensation, which is followed by erythema and edema. Occasionally, papular and nodular eruptions may be seen first. Typically, a tender or mildly pruritic cellulitislike eruption occurs. Systemic symptoms, including asthma, arthralgia, and fever, may be evident, although they usually do not occur.
The clinical presentation can vary widely and may include the following:
- Annular plaques
- Vesicles and bullae - Bullous Wells syndrome associated with non-Hodgkin lymphoma16
- Urticaria17
- Edema
- Papules or nodules
Physical
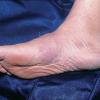
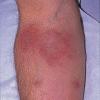
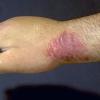
The lesions progress over a few days to become large, indurated plaques of edema and erythema, with violaceous edges and no calor. The lesions may last for several weeks, but they gradually darken from bright red to slate blue. Complete resolution with no scarring is typical, although scarring alopecia may occur.
The plaques can occur anywhere on the skin, and they may be solitary or multiple. Plaques on the affected areas are known to recur, and vesiculobullae may develop over the surface.
The clinical features seem to depend on the location of the infiltrates in the dermis. This observation suggests that a spectrum of eosinophilic dermatoses occurs in Wells syndrome.
Causes
The etiology is unknown. Wells syndrome is usually sporadic, but some familial cases have been described. Suggested precipitating factors include the following:
- Arthropod bites and stings, including those of the honeybee18
- Cutaneous viral infections
- Cutaneous parasitic infestations, including toxocariasis,19,20 ascariasis,21 and onchocerciasis22
- Leukemia
- Myeloproliferative disorders
- Atopic dermatitis
- Fungal infections
- Hypersensitivity reactions to medications
- Churg-Strauss syndrome: This syndrome has been associated in a few patients. These reports are noteworthy for the presence of bullae and of antineutrophil cytoplasmic antibodies.
Laboratory Studies
Peripheral blood and bone marrow eosinophilia are usually present. In peripheral blood, an increase in eosinophil cation protein (ECP) and IL-5 levels can be detected. Of note, the levels of ECP and IL-5 seem to be correlated with the severity of the disease.
Procedures
Eosinophilic cellulitis is usually diagnosed on the basis of the characteristic histopathologic findings in a skin biopsy specimen.
Histologic Findings
Skin biopsy specimens show a dermal infiltrate of eosinophils, histiocytes, and eosinophil debris between collagen bundles that forms flame figures. During the acute early phase, the dense infiltrate of degranulating eosinophils is usually located in the epidermis and the dermis, although it occasionally extends into the subcutaneous tissue and the underlying muscle.24,25,26
Vesiculation can occur. The blisters contain eosinophils and are predominately subepidermal and, occasionally, multiloculated and spongiotic. The location of the infiltrate is correlated with the different clinical features.
After weeks, the flame figures are seen, along with a palisade of histiocytes and giant cells around some collagen fibers. With immunofluorescent stains, eosinophil major basic protein is identified in the granules of the flame figures.27 On electron microscopy, the collagen fibers are intact; this finding suggests that an initial degeneration of collagen is not a factor in initiating the formation of flame figures.
Although the histopathologic findings of eosinophilia, histiocytes, and flame figures are characteristic of Wells syndrome, they are also found in other conditions, including bullous pemphigoid, eczema, tinea infection, and insect bites.
Medical Care
Numerous treatment options include the use of topical corticosteroids, griseofulvin, H1 antihistamines, cyclosporine, dapsone, and systemic corticosteroids.29 Systemic corticosteroids are the most effective treatment, but they may lead to corticosteroid dependence.
Medication
The goals of pharmacotherapy are to reduce morbidity and to prevent complications.
Antifungal
Mechanism of action usually involves inhibiting pathways (enzymes, substrates, transport) necessary for sterol/cell membrane synthesis or altering the permeability of the cell membrane (polyenes) of the fungal cell.
Griseofulvin (Fulvicin P/G, Grifulvin V)
Fungistatic activity. Fungal cell division is impaired by interfering with microtubules. Binds to keratin precursor cells. Keratin is gradually replaced by noninfected tissue, which is highly resistant to fungal invasions.
Adult
500 mg microsize (330-375 mg ultramicrosize) PO qd or bid, continue for 2 wk after clinical lesions resolve
Pediatric
Suggested dose: 20 mg microsize/kg/d (5 mg/lb/d) PO or 7.3 mg ultramicrosize/kg/d (3.3 mg/lb/d) PO
Reduced effects of cyclosporine, salicylates, and warfarin (decreased hypoprothrombinemic activity); avoid alcohol use because disulfiramlike reaction may occur; intense UV light exposure may result in phototoxic reaction; contraceptives may lose their effectiveness
Documented hypersensitivity; hepatic injury
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Better absorption when taken with fatty food; adverse effects may include abdominal pain, nausea, diarrhea, headache and, rarely, Stevens-Johnson syndrome and photodermatitis; 20% of patients experience adverse effects; in prolonged therapy, observe patients closely; monitor renal, hepatic, and hematopoietic function regularly
Antibiotics
Therapy must cover all likely pathogens in the context of this clinical setting.
Dapsone (Avlosulfon)
Bactericidal and bacteriostatic against mycobacteria; mechanism of action is similar to that of sulfonamides where competitive antagonists of PABA prevent formation of folic acid, inhibiting bacterial growth.
Adult
50-300 mg PO qd
Pediatric
Not established
May inhibit anti-inflammatory effects of clofazimine; hematologic reactions may increase with folic acid antagonists, eg, pyrimethamine (monitor for agranulocytosis during second and third months of therapy); probenecid increases toxicity; trimethoprim with dapsone may increase toxicity of both drugs; because of increased renal clearance, levels may significantly decrease when administered concurrently with rifampin
Documented hypersensitivity; known G-6-PD deficiency
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Perform weekly blood counts (first mo), then monthly WBC counts (6 mo), then semiannually thereafter; discontinue if significant reduction in platelets, leukocytes, or hematopoiesis; caution in methemoglobin reductase deficiency, G-6-PD deficiency (patients receiving >200 mg/d), or hemoglobin M because of high risk for hemolysis and Heinz body formation; caution in patients exposed to other agents or conditions (eg, infection, diabetic ketosis) capable of producing hemolysis; peripheral neuropathy can occur (rare); phototoxicity may occur when exposed to UV light
Immunosuppressants
These agents inhibit key factors in the immune system responsible for immune reactions.
Cyclosporine (Sandimmune, Neoral)
Demonstrated to be helpful in a variety of skin disorders.
Adult
2.5-5 mg/kg/d PO in divided doses
Pediatric
Administer as in adults
Carbamazepine, phenytoin, isoniazid, rifampin, and phenobarbital may decrease concentrations; azithromycin, itraconazole, nicardipine, ketoconazole, fluconazole, erythromycin, verapamil, grapefruit juice, diltiazem, aminoglycosides, acyclovir, amphotericin B, and clarithromycin may increase toxicity; acute renal failure, rhabdomyolysis, myositis, and myalgias increase when taken concurrently with lovastatin; methylprednisolone and cyclosporine mutually inhibit one another, resulting in increased plasma levels of each drug
Documented hypersensitivity; uncontrolled hypertension or malignancies; do not administer concomitantly with PUVA or UV-B radiation in psoriasis because it may increase risk of cancer
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Evaluate renal and liver functions often by measuring BUN, serum creatinine, serum bilirubin, and liver enzyme levels; may increase risk of infection and lymphoma; reserve IV use only for those who cannot take PO
Cortisone (Cortone)
Decreases inflammation by suppressing migration of polymorphonuclear leukocytes and reversing increased capillary permeability.
Adult
25-300 mg/d PO/IM divided q12-24h
Pediatric
0.5-0.75 mg/kg/d PO/IM or 20-25 mg/m2/d divided q8h
Alternative IM administration: 0.25-0.35 mg/kg/d IM qd or 12.5 mg/m2/d
Estrogen coadministration may increase corticosteroid levels; may increase digitalis toxicity secondary to hypokalemia
Documented hypersensitivity; viral, fungal, or tubercular skin lesions
Pregnancy
D - Fetal risk shown in humans; use only if benefits outweigh risk to fetus
Precautions
Caution in patients with hyperthyroidism, cirrhosis, nonspecific ulcerative colitis, osteoporosis, peptic ulcer, diabetes, and myasthenia gravis
Prednisone (Orasone, Meticorten, Sterapred, Deltasone)
May decrease inflammation by reversing increased capillary permeability and suppressing PMN activity.
Adult
5-60 mg/d PO qd or divided bid/qid; taper over 2 wk as symptoms resolve
Pediatric
4-5 mg/m2/d PO; alternatively, 0.05-2 mg/kg PO divided bid/qid; taper over 2 wk as symptoms resolve
Coadministration with estrogens may decrease clearance; concurrent use with digoxin may cause digitalis toxicity secondary to hypokalemia; phenobarbital, phenytoin, and rifampin may increase metabolism of glucocorticoids (consider increasing maintenance dose); monitor for hypokalemia with coadministration of diuretics
Pregnancy
B - Fetal risk not confirmed in studies in humans but has been shown in some studies in animals
Precautions
Abrupt discontinuation of glucocorticoids may cause adrenal crisis; hyperglycemia, edema, osteonecrosis, myopathy, peptic ulcer disease, hypokalemia, osteoporosis, euphoria, psychosis, myasthenia gravis, growth suppression, and infections may occur with glucocorticoid use
Hydrocortisone topical (LactiCare-HC, Cortaid, Dermacort, Westcort, CortaGel)
An adrenocorticosteroid derivative suitable for application to skin or external mucous membranes. Decreases inflammation by suppression of migration of polymorphonuclear leukocytes and reversal of increased capillary permeability.
Adult
Apply sparingly to affected areas bid/qid
Pediatric
Apply as in adults
Documented hypersensitivity; viral, fungal, and bacterial skin infections
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Prolonged use, applying over large surface areas, applying potent steroids, and use of occlusive dressings may increase systemic absorption of corticosteroids and may cause Cushing syndrome, reversible HPA-axis suppression, hyperglycemia, and glycosuria
Dexamethasone (Alba-Dex, Dexone, Baldex, AK-Dex, Decadron)
For various allergic and inflammatory diseases. Decreases inflammation by suppressing migration of polymorphonuclear leukocytes and reducing capillary permeability.
Adult
0.75-9 mg/d IV/IM in divided doses q6-12h
Pediatric
0.08-0.3 mg/kg/d IV/IM or 2.5-10 mg/m2/d IV/IM divided q6-12h
Effects decrease with coadministration of barbiturates, phenytoin, and rifampin; decreases effect of salicylates and vaccines used for immunization
Documented hypersensitivity; active bacterial or fungal infection
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Increases risk of multiple complications, including severe infections; monitor adrenal insufficiency when tapering; abrupt discontinuation of glucocorticoids may cause adrenal crisis; hyperglycemia, edema, osteonecrosis, myopathy, peptic ulcer disease, hypokalemia, osteoporosis, euphoria, psychosis, myasthenia gravis, growth suppression, and infections are possible complications of glucocorticoid use
Betamethasone (Topical) (Diprolene, Maxivate, Alphatrex)
For inflammatory dermatoses responsive to steroids. Decreases inflammation by suppressing migration of polymorphonuclear leukocytes and reversing capillary permeability. Affects production of lymphokines and has inhibitory effect on Langerhans cells.
Adult
Apply thin film bid/qid until response
Pediatric
Apply as in adults with caution
Documented hypersensitivity; paronychia; cellulitis; impetigo; angular cheilitis; erythrasma; erysipelas; rosacea; perioral dermatitis; acne
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Do not use in skin with decreased circulation; can cause atrophy of groin, face, and axillae; may cause striae distensae or rosacealike eruption; may increase skin fragility; rarely may suppress HPA axis; if infection develops and is not responsive to antibiotic treatment, discontinue until infection is controlled; do not use monotherapy to treat widespread plaque psoriasis
H1 receptor antagonists
These agents act by competitive inhibition of histamine at the H1 receptor. This mediates the wheal and flare reactions, bronchial constriction, mucous secretion, smooth muscle contraction, edema, hypotension, CNS depression, and cardiac arrhythmias.
Cyproheptadine (Periactin)
For the symptomatic relief of allergic symptoms caused by histamine released in response to allergens and skin manifestations.
Adult
4-20 mg PO qd, not to exceed 0.5 mg/kg/d; initiate therapy with 4 mg tid; dose range is 12-16 mg/d and occasionally up to 32 mg/d
Pediatric
Calculate total daily dose as 0.25 mg/kg (0.11 mg/lb) or 8 mg/m2
2-6 years: 2 mg PO bid/tid; not to exceed 12 mg/d
7-14 years: 4 mg PO bid/tid; not to exceed 16 mg/d
>14 years: Administer as in adults
Potentiates effects of CNS depressants; MAOIs may prolong and intensify anticholinergic and sedative effects of antihistamines
Documented hypersensitivity; narrow-angle glaucoma; stenosing peptic ulcer; symptomatic prostatic hypertrophy; bladder neck obstruction; pyloroduodenal obstruction; lower respiratory tract symptoms
Pregnancy
B - Fetal risk not confirmed in studies in humans but has been shown in some studies in animals
Precautions
Caution in patients with a predisposition to urinary retention, history of bronchial asthma, increased intraocular pressure, hyperthyroidism, cardiovascular disease, or hypertension; may thicken bronchial secretions caused by anticholinergic properties and may inhibit expectoration and sinus drainage
Diphenhydramine (Benylin, Benadryl)
For symptomatic relief of symptoms caused by release of histamine in allergic reactions.
Adult
25-50 mg PO q6-8h prn; not to exceed 400 mg/d
10-50 mg IV/IM q6-8h prn; not to exceed 400 mg/d
Pediatric
12.5-25 mg PO tid/qid; not to exceed 300 mg/d
5 mg/kg/d IV/IM or 150 mg/m2/d IV/IM divided qid; not to exceed 300 mg/d
28


