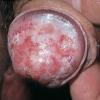 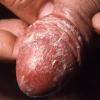 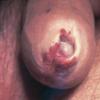 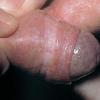
Balanitis xerotica obliterans
Lichen sclerosus is a chronic, progressive, sclerosing inflammatory dermatosis of unclear etiology. Most reported lichen sclerosus cases (83%) involve the genitalia. In men, this genital involvement has traditionally been known as balanitis xerotica obliterans (BXO). A more accurate term is male genital or penile lichen sclerosus. The image below shows the condition.
Yardley et al1 believe that the prevalence of BXO is greater than previous series have shown and that it may manifest in children at an earlier age than previous series have shown. This belief is based on a study of 422 boys at a median age of 6 years 2 months (range, 3 mo to 16 y), of whom 186 (44.1%) received treatment involving surgery (148 circumcision, 33 preputial adhesiolysis, 5 frenuloplasty). Of the 186 boys, 110 had histological tissue examination; 84.8% of skin samples were pathologic. Specifically, tissue showed chronic inflammation (n = 69; 46.6%), BXO (n = 51; 34.5%), and fibrosis (n = 4; 2.7%).
Related eMedicine articles include Lichen Sclerosus et Atrophicus, Balanitis Circumscripta Plasmacellularis, and Balanitis.
Pathophysiology
The etiology of male genital lichen sclerosus is unknown, but it is thought to be multifactorial. Balanitis xerotica obliterans (BXO) has occurred in monozygotic twins, which suggests a genetic basis for the disease in some cases. Human papillomavirus type 6 or type 16 has not been detected in patients with BXO, which strongly suggests that genital papillomaviruses do not have a strong association with BXO.
History
Early in its course, penile lichen sclerosus (balanitis xerotica obliterans [BXO]) is relatively asymptomatic with only mild visually observable changes of the penis and glans. Physical changes occur over months or years and may include color or textural changes. Early symptoms are more prevalent in uncircumcised patients.
- Symptoms occurring with time and progression of penile lichen sclerosus are as follows:
- Pruritus
- Burning
- Hypoesthesia of the glans penis
- Dysuria
- Painful erection with altered sexual function
- Decrease in urinary force or stream caliber
- Urethritis with or without discharge
- Symptoms occurring in late penile lichen sclerosus (in uncircumcised patients) are as follows:
- Phimosis (inability to retract the foreskin over the glans)
- Paraphimosis (inability to return an already retracted foreskin back over the glans)
- The development of multifocal squamous cell carcinoma (SCC) in persons with lichen sclerosus et atrophicus of the penis and hepatitis C virus infection has been reported. SCC of the penis arising from BXO alone has also been noted.
- A urethral stone manifesting as a stop valve, a rare complication of BXO, has been reported.
Physical
Early penile lichen sclerosus (balanitis xerotica obliterans [BXO]) demonstrates only subtle physical findings (eg, mild, nonspecific erythema; mild hypopigmentation).
- As the condition progresses, single or multiple discrete erythematous papules or macules progress and coalesce into atrophic ivory, white, or purple-white patches or plaques.
- Lesions most commonly affect the glans and prepuce.
- The frenulum, urethral meatus, fossa navicularis, penile shaft, and perianal areas may become involved.
- A sclerotic white ring at the tip of the prepuce is diagnostic at this stage.
- Erosions, fissures, petechiae, serous and hemorrhagic bullae, and telangiectasias of the glans have been reported, albeit uncommonly.
- With further disease progression, the glans may become adherent to the prepuce.
- The coronal sulcus and frenulum may be sclerotically destroyed.
- The urethral meatus may narrow to the point of urinary retention.
- Urinary retention may be severe enough to cause retrograde damage to the posterior urethra and to the bladder and kidneys.
- Significant urethral meatal narrowing has led to sloughing of the distal half centimeter of the urethra.
- Phimosis and paraphimosis of uncircumcised patients may occur at this late stage.
- Seventeen percent of lichen sclerosus cases are extragenital, beginning as mild, nonspecific erythema with mild hypopigmentation.
- In one case report8 , BXO in a middle-aged man involved the entire anterior urethra and the scrotum. It manifested as a palpable nodular scrotal mass and caused obstructive voiding symptoms. He was treated with a staged urethroplasty.
Causes
The etiology of male genital lichen sclerosus (balanitis xerotica obliterans [BXO]) is unknown but is thought to be multifactorial. Several contributing factors are possible, as follows:
- Circumcision after age 13 years/uncircumcised state
- This may very well be due to the effect known as the isomorphic, or Koebner, phenomenon. The large majority of inflammatory dermatoses of the male genitalia, including lichen sclerosus, occur in uncircumcised or late-circumcised men.
- The presence of a foreskin may promote chronic irritation or serve to maintain a friendly environment for an as-yet unidentified infectious agent. Such chronic irritation and subsequent inflammation may initiate the changes noted in lichen sclerosus.
- Hormonal factors
- Hormonal influences in the development of lichen sclerosus have long been postulated, mainly in female vulvar lichen sclerosus.
- Most studies have concentrated on the role of testosterone in the pathogenesis of vulvar lichen sclerosus. Childhood vulvar lichen sclerosus frequently resolves with the onset of menarche and the related pubertal increase in testosterone production in genital skin; additionally, adults with lichen sclerosus have been found to have decreased serum levels of free testosterone, androstenedione, and dihydrotestosterone compared with control subjects.
- The underlying defect may be a problem with the function of the enzyme 5-alpha reductase.
- Autoimmune disease
- Various autoantibodies (including antinuclear, thyroid antimicrosomal, antigastric parietal cell, anti-adrenal cortex, antismooth muscle, and antimitochondrial antibodies) have been detected in patients with lichen sclerosus.
- Vitiligo, thyroid disease, diabetes, and alopecia areata have also been commonly reported in association with lichen sclerosus.
- Genetic factors
- Lichen sclerosus (not necessarily genital lichen sclerosus) has been reported in families, including twins (identical and nonidentical), sisters, mothers and daughters, and a brother and sister.
- Note, however, that no consistent pattern of genetic inheritance has been identified.
- Presence of human papillomaviruses
- The presence of human papillomaviruses (HPV) has been reported in some cases of childhood penile lichen sclerosus. Whether the lichen sclerosus is directly attributable to HPV infection, or if lichen sclerosus merely promotes HPV infection is unclear.
- Patients with penile lichen sclerosus alone have not been demonstrated to have a higher incidence of HPV infection.
- Other: In a study of 18 patients9 with combined buccal mucosa grafting and genital skin flap reconstruction of extensive anterior urethral strictures, 16.7% of stricture cases were caused by BXO.
Differential Diagnoses
Balanitis Circumscripta Plasmacellularis
|
Reactive Arthritis
|
Candidiasis, Mucosal
|
Vitiligo
|
Erythroplasia of Queyrat (Bowen Disease of the Glans Penis)
|
|
Lichen Planus
|
|
Psoriasis, Plaque
|
|
Other Problems to Be Considered
Phimosis
Balanitis
Buried penis
Zoon plasma cell balanitis
Pseudoepitheliomatous keratotic and micaceous balanitis
Pseudoepitheliomatous keratotic and micaceous balanitis (PKMB) is a very rare papulosquamous dermatosis of the glans penis. PKMB presents in elderly, uncircumcised men as a slowly growing, coarsely scaling, micaceous, white-to-gold, laminated, well-demarcated plaque. The lesion may grow to involve the coronal sulcus and the distal penile shaft. Symptoms include phimosis, pain, and interference with sexual activity. PKMB is considered to be a premalignant condition. Nearly all reported patients have had malignant degeneration. Reported associated malignancies include SCC, verrucous carcinoma, and fibrosarcoma.
Laboratory Studies
- A rapid protein reagin test helps exclude syphilis.
Procedures
- Skin biopsy aids in the diagnosis of male genital lichen sclerosus (balanitis xerotica obliterans [BXO]).
Histologic Findings
Histopathologic changes of genital lichen sclerosus are similar to those of nongenital lichen sclerosus.
Epidermal findings include orthokeratosis, hyperkeratosis with follicular plugging, hyperkeratosis without follicular plugging, stratum malpighii atrophy, basal layer hydropic degeneration, and dermoepidermal clefting (in some cases).
Follicular plugging is not apparent in mucosal BXO. Significant dermal edema and homogenization of the collagen in the upper dermis occurs, with dilatation of blood and lymph vessels and a loss of elastic fibers.
The immune cells moving into areas of BXO include lymphocytes, plasma cells, and histiocytes in the mid dermis. The inflammatory infiltrate is less pronounced in long-standing lesions.
Medical Care
- No consistently effective treatment has been developed for penile lichen sclerosus (balanitis xerotica obliterans [BXO]); however, the following therapies have varying degrees of reported success:
- Topical and intralesional steroids: Topical steroids can offer a reliable option only in the management of mild BXO limited to the prepuce in boys with minimal scar formation. Patients and their families must have realistic expectations with regard to the success of such treatments. Steroid-based creams are ineffective in persons with established scarring. Studies have shown that applying a potent topical steroid improves BXO in the histologically early and intermediate stages of disease and may inhibit further worsening in the late stages. Kiss10 questioned the utility of topical steroid-based creams for the treatment of clinical BXO. Differences in success rates may relate to an unwillingness to use superpotent corticosteroids.
- Topical steroids and skin stretching: Ghysel et al reported on successful therapy with topical steroid application and skin stretching on prepubertal boys with unretractable foreskin and phimosis.11
- Tacrolimus: Successful treatment of BXO with topical tacrolimus has been reported.
- Etretinate (no longer available): Acitretin is the current equivalent.
- Carbon dioxide laser treatment12
- Ebert et al,13 in a retrospective analysis of 13 children with BXO published in 2007, reported that the relapse rate was lower after topical tacrolimus therapy than with betamethasone therapy.
- In a case series of 3 patients, 2 had softening of the skin and pruritus, tenderness, and inflammatory change resolution within 3 weeks of receiving oral and intramuscular penicillin. Dirithromycin at 500 mg/d abated BXO in a third patient; the BXO returned when dirithromycin was discontinued but it improved again upon resumption of therapy.
- Further treatment, or treatment of circumcised patients, is more challenging.
Surgical Care
A variety of surgical techniques can be used to treat more severe penile lichen sclerosus (balanitis xerotica obliterans [BXO]).
- Uncircumcised patients usually benefit from therapeutic circumcision. Provide regular follow-up care to observe any changes in involved areas suggestive of malignancy.
- Consider surgical intervention for symptoms or signs of urethral meatal stenosis.
- Dubey et al14 report that in BXO-related strictures with a viable urethral plate, 1-stage dorsal onlay buccal mucosal urethroplasty achieves superb medium-term results. They also state that the intervention created a normal, wide-caliber, slitlike glans, and a 2-stage procedure provides effective treatment but is associated with a higher revision rate.
- Full-thickness skin grafts from eyelids to penis, plus split-thickness grafts in chronic BXO have been reported.
- Buccal mucosa appears to be a durable source of nongenital tissue for urethral replacement. Attention to detail in terms of graft harvest, graft preparation, and graft fixation helps to avoid major postoperative complications. Onlay grafts appear to be preferable to tube grafts, and patients with a diagnosis of BXO do not appear to be candidates for the 1-stage urethral reconstruction using buccal mucosa.
- Circumferential laser vaporization for severe meatal stenosis secondary to BXO reportedly is effective.
- In 2007, Levine et al15 reported on buccal mucosa graft urethroplasty for anterior urethral stricture repair. They evaluated the impact of stricture location and lichen sclerosus on surgical outcome. When lichen sclerosus affects the penis, complete excision of the diseased urethra with multistage repair decreases the rate of stricture recurrence associated with a 1-stage repair.
- Palminteri et al16 treated 17 patients, performing y resurfacing or reconstruction of the glans penis for benign, premalignant, and malignant penile lesions (5 glans skinning and resurfacing; 5 glans amputation and reconstruction of the neoglans, and 7 partial penile amputation and reconstruction of the neoglans). Four patients had lichen sclerosus. Glans resurfacing and reconstruction were performed with the use of a skin graft harvested from the thigh. Patients who received glans resurfacing reported glandular sensory restoration and complete sexual ability. Patients receiving glansectomy or partial penectomy with neoglans reconstruction maintained sexual function and activity, albeit with reduced sensitivity secondary to glans/penile amputation. Palminteri et al concluded that glans resurfacing or reconstruction can ensure a normal-appearing and functional penis, without jeopardizing cancer control.
Consultations
- Consider consultation with urologists for the following:
- Therapeutic circumcision
- Circumcision for symptomatic phimosis or paraphimosis
- Significant narrowing or obstruction of the urethral meatus or changes in urinary flow
Topical steroids, especially superpotent topical steroids, are the mainstay of medical therapy. Zavras et al reported successful treatment of 1079 (91.1%) of 1185 boys with a diagnosis of phimosis using fluticasone propionate 0.05%, including boys with mild balanitis xerotica obliterans (BXO).17
Topical testosterone is mostly ineffective and is not discussed further. Etretinate has been used with limited success but is no longer available for prescription in the United States.
Topical corticosteroids
Help reduce inflammatory lesions and may reduce or resolve lesions.
Clobetasol (Temovate)
Class I superpotent topical steroid; suppresses mitosis and increases synthesis of proteins that decrease inflammation and cause vasoconstriction. Used in most studies dealing with treatment of lichen sclerosus.
Adult
Apply to affected areas qd for up to 12 wk, although continuous treatment for >2 wk may begin to cause atrophic changes; atrophic changes will be more pronounced in genital area than other areas of the body; not to exceed 50 g/wk
Pediatric
Not established
Documented hypersensitivity; viral or fungal skin infections
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Steroid atrophy commonly occurs when superpotent topical steroids are used in genital area for even short periods; observe patients for any such changes; may suppress adrenal function in prolonged therapy
Topical immunomodulators
Topical calcineurin inhibitors are immune suppressants that block early T-cell activation, degranulation of mast cells, and multiple cytokines.
Tacrolimus ointment 0.1% or 0.03% (Protopic)
Mechanism of action in atopic dermatitis is not known. Reduces itching and inflammation by suppressing release of cytokines from T cells. Also inhibits transcription for genes that encode IL-3, IL-4, IL-5, GM-CSF, and TNF-alpha, all of which are involved in early stages of T-cell activation. Additionally, may inhibit release of preformed mediators from skin mast cells and basophils and may down-regulate expression of FCeRI on Langerhans cells. Can be used in patients >2 y. More expensive than topical corticosteroids. Available as ointment in concentrations of 0.03 and 0.1%. Indicated only after other treatment options have failed.
Adult
Apply thin layer to affected skin areas bid and rub in gently and completely; continue treatment for 1 wk after clearing of signs and symptoms
Short-term and intermittent use only
Pediatric
<2 years: Not established
2-15 years: Apply 0.03% ointment bid to affected area(s)
>15 years: Administer as adults
Short-term and intermittent use only
None if no systemic absorption occurs
Documented hypersensitivity to tacrolimus or components of ointment
Pregnancy
C - Fetal risk revealed in studies in animals but not established or not studied in humans; may use if benefits outweigh risk to fetus
Precautions
Do not use with occlusive dressings; may be associated with an increased risk of folliculitis in adults; may cause local burning sensation, stinging, soreness, or pruritus (typically improves as lesions heal); for external use only; minimize exposure to natural or artificial sunlight (eg, tanning beds or UVA/B treatment); be sure skin is completely dry before application
The product insert for tacrolimus was revised in January 2006 and contains a boxed warning stating the long-term safety of calcineurin inhibitors has not been established. Although a causal relationship has not been established, rare cases of malignancy (eg, skin and lymphoma) have been reported. Only the 0.03% ointment is indicated for use in children aged 2-15 y.
|

