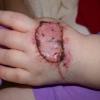
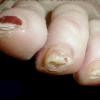
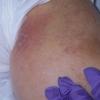
Aspergillosis
Aspergillus species are ubiquitous molds found in organic matter. Although more than 100 species have been identified, the majority of human illness is caused by Aspergillus fumigatus and Aspergillus niger and, less frequently, by Aspergillus flavus and Aspergillus clavatus. The transmission of fungal spores to the human host is via inhalation. Also see the eMedicine articles Aspergillosis (dermatology focus), Aspergillosis (pediatric focus), and Aspergillosis, Thoracic (radiology focus).
Aspergillus may cause a broad spectrum of disease in the human host, ranging from hypersensitivity reactions to direct angioinvasion. Aspergillus primarily affects the lungs, causing 4 main syndromes, including allergic bronchopulmonary aspergillosis (ABPA), chronic necrotizing Aspergillus pneumonia (or chronic necrotizing pulmonary aspergillosis [CNPA]), aspergilloma, and invasive aspergillosis. However, in patients who are severely immunocompromised, Aspergillus may hematogenously disseminate beyond the lung, potentially causing endophthalmitis, endocarditis, and abscesses in the myocardium, kidney, liver, spleen, soft tissue, and bone. Aspergillus is second to Candida species as a cause of fungal endocarditis. Aspergillus -related endocarditis and wound infections occur in the context of cardiac surgery.
ABPA is a hypersensitivity reaction to A fumigatus colonization of the tracheobronchial tree and occurs in conjunction with asthma and cystic fibrosis (CF). Allergic fungal sinusitis may also occur alone or with ABPA. Bronchocentric granulomatosis and malt worker's lung are 2 hypersensitivity lung diseases that are caused by Aspergillus species, but they are rare.
An aspergilloma is a fungus ball (mycetoma) that develops in a preexisting cavity in the lung parenchyma. Underlying causes of the cavitary disease may include treated tuberculosis or other necrotizing infection, sarcoidosis, CF, and emphysematous bullae. The ball of fungus may move within the cavity but does not invade the cavity wall; however, it may cause hemoptysis.
CNPA is a subacute process usually found in patients with some degree of immunosuppression, most commonly that associated with underlying lung disease, alcoholism, or long-term corticosteroid therapy. Because it is uncommon, CNPA often remains unrecognized for weeks or months and can cause a progressive cavitary pulmonary infiltrate.
Invasive aspergillosis is a rapidly progressive, often fatal infection that occurs in patients who are severely immunosuppressed, including those who are profoundly neutropenic, those who have received bone marrow or solid organ transplants, and patients with advanced AIDS1 or chronic granulomatous disease. This infectious process is characterized by invasion of blood vessels, resulting in multifocal infiltrates, which are often wedge-shaped, pleural-based, and cavitary. Dissemination to other organs, particularly the central nervous system, may occur
Aspergillus causes a spectrum of disease, from colonization to hypersensitivity reactions to chronic necrotizing infections to rapidly progressive angioinvasion, often resulting in death. Rarely found in individuals who are immunocompetent, invasive Aspergillus infection almost always occurs in patients who are immunosuppressed by virtue of underlying lung disease, immunosuppressive drug therapy, or immunodeficiency.
Aspergillus hyphae are histologically distinct from other fungi in that the hyphae have frequent septae, which branch at 45° angles. The hyphae are best visualized in tissue with silver stains. Although many species of Aspergillus have been isolated in nature, A fumigatus is the most common cause of infection in humans. A flavus and A niger are less common. Likely, this relates to the ability of A fumigatus, but not most other Aspergillus species, to grow at normal human body temperature.
Human host defense against the inhaled spores begins with the mucous layer and the ciliary action in the respiratory tract. Macrophages and neutrophils encompass, engulf, and eradicate the fungus. However, many species of Aspergillus produce toxic metabolites that inhibit macrophage and neutrophil phagocytosis. Corticosteroids also impair macrophage and neutrophil function. Underlying immunosuppression (eg, HIV disease, chronic granulomatous disease, pharmacologic immunosuppression) also contributes directly to neutrophil dysfunction or decreased numbers of neutrophils. In individuals who are immunosuppressed, vascular invasion is much more common and may lead to infarction, hemorrhage, and necrosis of lung tissue. Persons with CNPA typically have granuloma formation and alveolar consolidation. Hyphae may be observed within the granulomata
Invasive aspergillosis rarely occurs in patients who are immunocompetent.
- ABPA is found in people with asthma and/or CF who are allergic to Aspergillus. The thick mucus found in the airways of these patients may make clearing inhaled Aspergillus spores difficult. Additionally, evidence of genetic susceptibility has been reported. Patients who have certain HLA alleles, particularly HLA-DR2, have increased susceptibility to ABPA, whereas HLA-DQ2 appears to be protective.4
- Risk factors involved in the development of CNPA include underlying pulmonary disease (including COPD, interstitial lung disease, and previous thoracic surgery) and altered immune status due to chronic corticosteroid therapy, alcoholism, collagen-vascular disease, or chronic granulomatous disease.
- Aspergilloma typically develops in the context of preexisting cavitary disease. Aspergillomas may develop in patients with invasive aspergillosis or chronic necrotizing Aspergillus pneumonia.
Invasive aspergillosis occurs almost exclusively in patients who are immunocompromised.
- Neutropenia and corticosteroid therapy are major risk factors.
- In addition to patients who have undergone transplantation, patients profoundly neutropenic after receiving chemotherapy for hematologic malignancies or lymphoma, children with chronic granulomatous disease, and patients with late-stage HIV disease also are at risk.
- Specific risk factors for invasive aspergillosis after bone marrow transplantation include prolonged neutropenia, graft versus host disease, high-dose corticosteroid therapy, disruption of normal mucosal barriers, mismatched or unrelated donor transplants, and the presence of central venous catheters.
- Invasive Aspergillus infection in patients without malignancy or prior chemotherapy (who probably are nevertheless not immunocompetent) is most commonly seen in those with critical illness and COPD who are taking long-term corticosteroid therapy
Laboratory Studies
Because Aspergillus infection may cause colonization, allergy, or invasive infection, its manifestations are quite variable and are best considered based on the disease process.
Allergic bronchopulmonary aspergillosis (ABPA) is defined by several abnormalities, including asthma, eosinophilia, a positive skin test result for A fumigatus, marked elevation of the serum immunoglobulin E (IgE) level to greater than 1000 IU/dL, fleeting pulmonary infiltrates, central bronchiectasis, mucoid impaction, and positive test results for Aspergillus precipitins (primarily immunoglobulin G [IgG], but also immunoglobulin A and immunoglobulin M, antibodies). Minor criteria for diagnosis include positive Aspergillus radioallergosorbent assay test results and culture findings for Aspergillus in sputum.
Diagnostic criteria for ABPA in persons with CF were revised by the Cystic Fibrosis Foundation. ABPA is considered a definite diagnosis requiring treatment if the following are noted: (1) clinical deterioration, including cough, wheeze, increased sputum production, diminished exercise tolerance, or diminished pulmonary function; (2) total serum IgE level greater than 1000 IU/mL or a greater than 2-fold rise from baseline; (3) positive serology results for Aspergillus (Aspergillus precipitins or Aspergillus -specific IgG or IgE); and (4) new infiltrates on chest radiographs or CT scans. Treatment for ABPA is also recommended in patients with CF who have new radiographic findings and symptoms and a change in baseline IgE level to greater than 500 IU/mL.6
Definitive diagnosis of invasive aspergillosis or chronic necrotizing Aspergillus pneumonia depends on the demonstration of the organism in tissue.
In the appropriate clinical setting of pulmonary infiltrates in a patient who is neutropenic or immunosuppressed, visualization of the characteristic fungi using Gomori methenamine silver stain or Calcofluor or a positive culture result from sputum, needle biopsy, or bronchoalveolar lavage (BAL) fluid should result in the prompt institution of therapy. This is especially important after bone marrow transplantation because a positive Aspergillus culture result from sputum has a 95% positive predictive value for invasive disease. However, a negative fungus result from culture of sputum or BAL fluid does not exclude pulmonary aspergillosis because Aspergillus is cultured from sputum in 8-34% of patients and from BAL fluid in 45-62% of patients eventually found by biopsy or autopsy to have invasive disease.
An assay to detect galactomannan, a major component of the Aspergillus cell wall, is available.7 Patients who are at high risk, such as those who have received stem cell transplants or who have prolonged neutropenia, may be screened for the development of invasive Aspergillus infection by monitoring serum galactomannan levels weekly.8 The presence of an elevated galactomannan level in BAL fluid may also be helpful in the diagnosis of pulmonary aspergillosis in patients in whom compatible radiographic changes are present and BAL testing is performed in the suspicious area.9 A meta-analysis and systematic review determined that the measurement of BAL-galactomannan levels may help in diagnosing invasive aspergillosis early.
Aspergilloma does not cause many characteristic laboratory abnormalities. Aspergillus precipitin antibody test results (ie, for IgG) are usually positive
Treatment
Medical Care
The treatment of invasive aspergillosis and chronic necrotizing aspergillosis differs significantly from the treatment of allergic bronchopulmonary aspergillosis (ABPA) and aspergilloma.
Invasive aspergillosis
This is often rapidly progressive and has a high mortality rate; therefore, preventive therapy and rapid institution of therapy in patients in whom invasive aspergillosis is suggested may be lifesaving. Prophylactic antifungal therapy and the use of laminar airflow (LAF) or high-efficiency particulate air (HEPA) filtration of patient rooms in patients who receive bone marrow transplants and other high-risk patients may prevent invasive aspergillosis. In patients with solid organ transplants, especially lung, in whom Aspergillus is cultured from sputum without evidence of pneumonia (colonization), inhaled amphotericin B may be administered.
When high-risk patients develop a compatible clinical picture, empiric treatment for aspergillosis should be initiated as diagnostic testing is undertaken. Voriconazole is now considered the drug of choice for invasive aspergillosis because of better tolerance and improved survival with its use when compared with amphotericin.17 Posaconazole, amphotericin B, or amphotericin B lipid formulations may be considered as empiric therapy in critically ill patients if the clinical picture, particularly the presence of sinusitis, could be compatible with mucormycosis, because voriconazole is ineffective for Zygomycetes infection. Caspofungin has also been approved for treatment of invasive aspergillosis in patients who are unable to tolerate or are resistant to other therapies.18 Initial combination therapy is usually not indicated and should generally be reserved for treatment failures.19
If possible, the level of immunosuppression should be decreased. For example, patients who are neutropenic may receive growth factors (ie, granulocyte colony-stimulating factor, granulocyte-macrophage colony-stimulating factor), and patients with certain types of transplants, in which transplanted organ dysfunction will not be life threatening (eg, renal transplant), may have immunosuppressive medications, including corticosteroids, reduced or discontinued.
Combination antifungal therapy is sometimes used for patients whose disease progresses while on single-drug therapy. Concomitant therapy with azole antifungals and amphotericin is controversial because the azole antifungals decrease amphotericin-binding sites and may therefore diminish its effectiveness. Be alert to the possibility of diminished effectiveness of amphotericin in any patient who has received prior treatment with an azole antifungal, including voriconazole, itraconazole, fluconazole, or ketoconazole. Newer antifungal azoles are under study (eg, ravuconazole) and may be available for compassionate use in patients in whom other therapies have failed. Posaconazole, a new triazole, has been approved by the US Food and Drug Administration.20
Aspergilloma
Treatment is considered when patients become symptomatic, usually with hemoptysis. Surgical resection is curative but may not be possible in patients with limited pulmonary function. Oral itraconazole may provide partial or complete resolution of aspergillomas in 60% of patients. Successful intracavitary treatment, using CT-guided, percutaneously placed catheters to instill amphotericin alone or in combination with other drugs, including acetylcysteine and aminocaproic acid, has been reported in small numbers of patients.21
Bronchial artery embolization may be used for life-threatening hemoptysis in patients thought to have insufficient pulmonary reserve to tolerate surgery or in patients with recurrent hemoptysis (eg, patients with CF in whom hemoptysis may be related to underlying bronchiectasis with or without aspergilloma).22 Bronchial artery embolization requires a skilled and experienced radiologist because localizing the abnormal vessel(s) may be challenging. Because the anterior spinal arteries may originate from the bronchial vessels, serious neurologic complications, although rare, may occur.
Allergic bronchopulmonary aspergillosis
This is a hypersensitivity reaction that requires treatment with oral corticosteroids. Inhaled steroids are not effective.
Adding oral itraconazole to steroids in patients with recurrent or chronic ABPA may be helpful.23,24,25,26 This may allow more rapid resolution of infiltrates and symptoms, facilitating steroid tapering or lowering the needed maintenance corticosteroid dosage. In CF patients with ABPA, the concomitant use of itraconazole and inhaled corticosteroids may increase the risk of adrenal insufficiency.
Patients who have associated allergic fungal sinusitis benefit from surgical resection of obstructing nasal polyps and inspissated mucus in addition to corticosteroid therapy. Nasal washes with amphotericin or itraconazole have also been used.
Case reports have described the beneficial use of the anti-IgE monoclonal antibody omalizumab (Xolair) in patients with ABPA.27
Chronic necrotizing pulmonary aspergillosis
Treatment consists of therapy with voriconazole, or, in some cases, itraconazole (if expense is an issue), caspofungin, or amphotericin B or amphotericin lipid formulation. A prolonged course of therapy with the goal of radiographic resolution is needed. In addition, reduction or elimination of immunosuppression should be attempted, if possible.
Surgical resection may be considered when localized disease fails to respond to antifungal therapy.
Surgical Care
Invasive aspergillosis and CNPA
Surgical resection is a consideration for localized chronic necrotizing pulmonary aspergillosis (CNPA) that has failed to respond to prolonged antifungal therapy.28 Aspergillomas may occasionally form in areas of necrotizing pneumonia. These necrotic areas may bleed, sometimes massively, necessitating consideration of surgical resection. Patients may be high-risk surgical candidates because of underlying disease, coagulopathy, or thrombocytopenia and limited pulmonary reserve.
Aspergilloma
Surgical resection may be considered for massive hemoptysis if pulmonary function is sufficient enough for this sort of intervention. Assessment of operative risk necessitates obtaining pulmonary function studies, arterial blood gas determinations, and, possibly, split lung function studies (eg, quantitative perfusion lung scanning). Because aspergilloma occurs in cavitary areas, the affected lung may not be functional. Surgical resection may be difficult because of scarring, pleural adhesion, and the presence of abnormal vasculature.
Allergic bronchopulmonary aspergillosis
Areas of mucoid impaction may have a masslike appearance and are sometimes resected as an undiagnosed lung mass; however, steroid therapy and oral itraconazole therapy are preferred. Allergic fungal sinusitis usually requires endoscopic sinus surgery to improve drainage.
.


